Getting a Good Night’s Sleep
Table Of Contents
- Sleep Deprivation
- Tuning Out the Noise
- Dos and Don’ts for Getting a Good Night’s Sleep
- Nondrug Approaches for Falling Asleep
- Herbal Remedies for Sleep
- Medications and Insomnia
- Some Drugs That May Cause Insomnia
- Sleeping Pills
- Dependency and Withdrawal
- Over-the-Counter Sleep Medicine
- Sleep Apnea
- Cognitive Behavioral Therapy for Insomnia
- Recommended Health Guides
Sleep Deprivation
Are You an Insomniac?
Do you:
- find it regularly takes more than an hour to fall asleep?
- awaken in the early morning hours and can’t fall back asleep?
- have a hard time dragging yourself out of bed, even with an alarm clock?
- doze off during the day–while reading, traveling, listening to talks or watching television?
- have trouble concentrating? Is your short-term memory deteriorating?
- sleep a lot longer on weekends or while on vacation?
If you responded yes to one or more of these questions, you may be a chronic insomniac.
Insomnia affects an alarmingly large number of us: roughly half of all Americans sometimes have trouble falling asleep, and nearly 1 in 4 has chronic insomnia, according to National Sleep Foundation (NSF) poll data. Estimates from the Centers for Disease Control and Prevention put the number suffering from sleep or wakefulness disorders at around 50-70 million.
Doctors recommend that adults sleep for at least 7 or 8 hours a night. But a National Health Survey for 2005-2007 showed that nearly a third of us were sleeping less than 6 hours on average. The proportion of adults not getting enough sleep hovered right around 40% between 2013 and 2022, according to the CDC. Increasingly, children have joined the ranks of the sleepless: in 2009, nearly 70 percent of teens (who should sleep at least 9-10 hours) reported getting less than 8.
How Many of Us Aren’t Sleeping?
NSF poll data shows that 48% of Americans sometimes have trouble sleeping, while 22% are affected nearly every night. Women, older people, those suffering stress or anxiety, and drug and alcohol users are the most likely to suffer, but the problem has been widening to more and more of us, and has become a public health crisis.
Disturbed Sleep Isn’t the Same as Chronic Insomnia:
An occasional sleepless night isn’t so worrisome. Almost everyone has a hard time falling asleep once in awhile. Too much caffeine in the afternoon or evening can leave some of us wired for hours. A cold remedy with a decongestant can make it hard for an adult to fall asleep, and children may react to antihistamines by bouncing off the walls.
Emotional stress and other life disruptions can also make it hard to relax enough to get the rest we need. A breakup, problems at work, illness, and financial troubles can all interfere with a good night’s sleep. So can jet lag.
Most people get back on track once their lives return to normal. But others fall into a vicious cycle, and start having a hard time getting good shuteye each night. Instead of waking refreshed and ready to take on the world, they can barely get up, and struggle to remain alert throughout the day. Even folks who often stay up late by choice may find that their bodies begin to rebel.
Unfortunately, sleeping in on weekends doesn’t pay back our sleep debts. And it doesn’t take long for a lack of sleep to manifest in daytime drowsiness and fatigue. Short-term memory can be affected. Motor coordination and judgment may also suffer. The ability to drive, operate machinery, concentrate, and remember can all be impaired, and the risk of traffic accidents and falls increases.
Chronic sleep deprivation is also associated with high blood pressure, weight gain, diabetes, Alzheimer’s and reduced immunity, which can lead to a greater risk for cancer, among other things. The CDC considers insomnia a growing public health crisis.
People with insomnia can have a variety of sleeping problems. Some toss and turn all night. Others fall asleep fine but wake up in the early morning hours and can’t get back to sleep. But by far the most common complaint is difficulty falling asleep in the first place. If it regularly takes you more than an hour to drift off to dreamland, we’re talking serious insomnia.
Do We Really Need 8 Hours?
There is a counterargument. Some sleep experts believe we might not really need seven or eight hours straight of sleep after all. While chronic insomnia can certainly carry health risks, the notion that modern Westerners sleep considerably less than people of past eras may be false.
To study this, scientists looked at 3 contemporary hunter-gatherer societies, whose sleep habits haven’t changed much in thousands of years. They found that even people who aren’t exposed to cell phones, electricity, and the types of stresses that many Americans face daily don’t sleep very much: 6.5 hours per night, on average, which is actually a little less than us. And yet they tended to be healthy and fit (with energy outputs similar to ours).
So while being frequently sleep-deprived isn’t good for anyone, we may need to rethink how much shuteye we truly need in order to be healthy. As with so many things, quality may be more important than quantity.
Insomnia Risks
- sluggishness
- drowsiness
- forgetfulness
- delayed reaction time
- accidents
- falls
- mental impairment
- inefficiency
- mistakes
- nervousness
- high blood pressure
- weight gain
- digestive upset
- diabetes
- reduced immunity
- cancer
- Alzheimer’s
Tuning Out the Noise
Dr. Emmett Miller
Dr. Miller has produced some very relaxing audio and video materials. “Easing Into Sleep” may be especially helpful for insomniacs. Other favorites of ours include “Letting Go of Stress,” “Healing Journey,” “Rainbow Butterfly,” and the “Ten-Minute Stress Manager.”
You can order at: https://www.drmiller.com/
or by calling: 800-528-2737
It’s not uncommon for people with insomnia to complain that they have a hard time turning off their inner monologues. Their minds seem to go into overdrive the minute their heads hit the pillow. They relive events of the day, replay petty frustrations, dwell on problems, and generally worry themselves awake. These people often really benefit from learning how to relax, reduce their anxiety levels, and tune out the “thinkies.”
Strange as it may sound, some people report that setting aside time during the day specifically earmarked for worrying helps them calm down and quiet inner noise at night.
Relaxing with Music and Guided Meditation
An even better solution may be to listen to gentle music, meditation, or guided imagery. Our favorites are CDs or downloads by Dr. Emmett Miller. This physician, a founding father of the mind-body movement, has one of the most soothing voices we have ever heard. Listen to his “Easing into Sleep” as you’re getting ready for bed, and it will be hard not to let go of the day’s stresses and strains.
Unlike with sleep medication, there are no side effects! Ordering information is at the left, and you can also find him online.
Dos and Don’ts for Getting a Good Night’s Sleep
Avoid caffeine
Remember that coffee is just one source; caffeine appears in lots of things: tea, soft drinks, and of course energy drinks. But it can also appear in candies, as well as in powder form. And watch out for caffeine-contain- ing pain relievers, such as Anacin, BC Powder, Cope, Excedrin, Midol, Trigesic, and Vanquish. Some people are so sensitive to caffeine that they should avoid it after the morning, and it may help to cut it out completely.
Establish a pattern
Try to maintain a regular routine, going to sleep and getting up at the same times each night and day. (This means no sleeping in on weekends.) Don’t set yourself an unrealistically early bedtime, as this often backfires. Shifting sleep by an hour, as we do when changing from Daylight Savings Time to Standard Time or vice versa, can affect sleep negatively for as much as a week (Sleep Medicine Reviews, Aug., 2013).
Cautious napping
An afternoon snooze can be seductive. People who don’t suffer from chronic sleeping problems often benefit from catnaps. But sleeping during the day can make it harder to sleep at night, which leads to a vicious cycle. Try to make it through to bedtime and get a full night’s sleep.
Exercise regularly
We won’t tell you that farmers and lumberjacks never suffer from insomnia. But people who get lots of exercise often sleep well. Even a good, brisk walk can help. But timing is important; exercising too close to bedtime may actually make things worse, so try to fit your activity in at least a few hours before you’re ready to retire.
Take a hot bath
A hot bath raises the body’s core temperature. When you get out, your temperature falls, and this can trick your brain into thinking you’re already asleep (during sleep, body temperature drops). But again, timing is key. Plan on taking your 30-minute soak about an hour before bed.
Move the TV and avoid screens
It’s all too easy to get trapped by the TV or in an Internet spiral. Games, exciting movies, and annoying emails can get your heart rate up and keep you awake for hours. Many experts also believe that the blue light given off by our devices tricks our brain into thinking it’s daytime. And dozing off with the TV on may jolt you awake in the middle of the night. Take the TV out of your bedroom to eliminate temptation, and try to turn off all devices at least an hour before bed.
Turning off the devices and putting them away also applies for children and teens. A recent meta-analysis found that youngsters who had access to their tablets and smartphones in their bedrooms, even though they were ostensibly not using them, slept less well and were sleepier during the day (JAMA Pediatrics, online Oct. 31, 2016).
Avoid alcohol in the evening
Some people think a nightcap is a great way to fall asleep, but alcohol often actually makes sleeping problems worse by disrupting sleep cycles and melatonin levels. You may need to experiment to see whether a glass of wine at dinner has an impact on your sleep.
Relax before bed
Try to unwind before climbing into bed. Some folks find meditation helpful. A relaxing podcast or CD can be soothing before bedtime or once you’re settled in.
Give yourself a good sleep environment
Make sure that your bedroom is as comfortable and conducive to sleep as possible: not too hot or cold, not too bright or noisy. If light pollution is a problem, consider blackout curtains or a sleep mask. And if you can’t avoid noise, think about getting a white-noise machine, or even some good ear plugs, like the wax kind that swimmers use.
Change beds
If you can’t fall asleep in one bed, try moving. Sometimes just changing rooms can make a difference. There are even insomniacs who claim that switching to the floor can do the trick for them.
Do something mindless
If you’re tossing and turning for more than half an hour, get out of bed and do an activity that requires very little attention (and no electronic devices). For some, this may be reading a book. Others find knitting or doing word games or sudoku to be their lucky charms. After spending 20-30 minutes out of bed (or when you start getting sleepy), get back in bed and try again.
Eat a snack
Sometimes, a small bite at bedtime can help you drift off, even if you don’t have the munchies. Avoid energizing proteins and go instead for high-carb foods like Cheerios, graham crackers, or bananas 15 to 30 minutes before retiring. (For those with hypoglycemia, we have slightly different advice. Sometimes dips in blood sugar can wake you in the middle of the night. If that’s you, a protein boost may actually help you stay snoozing. Think peanut butter crackers, for example.)
Stay away from foods that cause heartburn
If heartburn is disturbing your sleep, you may want to avoid certain foods and drinks before hitting the hay. In addition to alcohol, coffee or espresso and caffeinated tea and soda, watch out for cheese, chocolate, fried or fatty foods, peppermint and tomatoes. If there are other foods that you know cause you trouble, you’ll want to avoid them after mid-afternoon.
Sex can be super
Some people find that sex is a wonderful way to help them fall asleep. It doesn’t work for everyone, but you may want to experiment to see if this is soporific for you.
Seek help from a professional
When all else fails, find an expert. A sleep lab at a medical center may be able to evaluate your sleeping patterns and come up with a successful strategy. Sleep counselors who offer cognitive behavioral therapy (CBT) are also very effective for some people. One study found CBT worked better than a prescription sleeping pill. Internet-based CBT for sleep has also been found to be effective for some people.
Nondrug Approaches for Falling Asleep
Readers’ Comments:
Shauna wrote:
“I am 35 years old. I have had difficulty sleeping since I came back from the military. I have tried everything!
“I thought I was destined for Ambien my whole life until I heard about 5-HTP. I have been using it for only a few days, but I can definitely feel the difference in my depression and overall mood.
“I haven’t given it have a chance to help me fall asleep yet, but I will try it without my Ambien this weekend. I take 200 mg of 5 HTP at night. It makes my tummy a little nauseous, but after that I’m fine. I’m hoping this will be the cure all.”
Another reader reported:
“My sleep pattern changed dramatically when I was about 50 years old. I fell asleep easily but woke after about 1-1/2 hours and took several hours to get back to sleep. That meant I was existing for years on 4-5 hrs of broken sleep a night.
“About 6 months ago I started taking 50 mgs of 5-HTP every morning and my sleep has improved tremendously. My understanding is that it tends to normalize serotonin and melatonin levels. When I ran out of 5-HTP for about a week, the old pattern returned, so now I make sure to always keep a supply on hand.”
Lucy in Flat Rock, NC, shared her experience with melatonin:
“Melatonin works amazingly well for me. I take it about an hour before bedtime and am able to go to sleep so easily and I sleep through the night and wake up feeling wonderful.
“If I don’t take it I have a very disrupted sleep, waking again and again, and lying awake for hours, and then feeling extremely tired the next day, sometimes while driving the car. I think melatonin makes me sleep and dream the way I did when I was young, before my insomnia problem arose.”
TD uses melatonin intermittently:
“I work an overnight shift 5 nights a week. I am home and ready to sleep between 7:30 & 8 am. I have found melatonin (3 mg) to be helpful in going into an immediate sleep. I rarely sleep more than 4 hours.
“I have found that melatonin seems to have no effect on my nights off, when I try to sleep like a normal person. So I really only use it for day-light sleeping, which is substituting for the melatonin that my body is not producing, as it is daytime.”
David in Hendersonville, NC, has a different solution:
“I thought I read the tart cherry juice was a good treatment for painful joints. Since my hip pain was keeping me up more frequently, I bought a jar and started drinking about 4 ounces at night before bed. Amazingly, the first night went by with no pain whatsoever! Now I drink the juice nearly every night and the results are quite consistent.”
Sleeping pills are a quick fix. They may work, but they can have side effects and lead to long-term risks. There are also many nondrug approaches to get a decent night’s sleep, and they seem worth a try.
Snacking to Sleep
Homer Simpson is famous for bedtime snacks. We fear that the chicken legs and potato chips he likes would probably keep you up. And there are other foods and drinks that you should avoid if you suffer from nighttime GERD (gastroesophageal reflux disease, or heartburn). Not uncommonly this condition makes it hard to fall asleep, or wakes people up in the middle of the night. It can feel like a heart attack, and that kind of pain should never be ignored.
But there are snacks that may actually improve your chances of drifting off. Neuroscientists have known for a long time that the amino acid tryptophan can help people sleep. It’s a building block for the brain chemical serotonin, known to be important in the sleep/wake cycle. The body also uses it to create melatonin, a hormone crucial for establishing our body clock.
Tryptophan
For years, tryptophan supplements were sold in pharmacies and health food stores. It was used for depression, jet lag, and PMS. Unfortunately, in 1989, disaster struck. People experienced weakness, muscle and joint pain, fever, rash, and shortness of breath. Blood tests revealed extremely high eosinophil counts (a type of white blood cell). Doctors labeled the strange condition eosinophilia-myalgia syndrome (EMS).
Soon, epidemiologists linked the EMS outbreak to tryptophan, and the supplement was pulled from the market. It’s now believed that most cases were caused by a bad batch out of Japan. Although the Food and Drug Administration (FDA) has never offered a complete explanation for the EMS tragedy, it’s unlikely that the agency will ever approve tryptophan. There’s no way to patent an amino acid, so it’s very unlikely that a drug company would be willing to undertake the high costs of testing it for safety and efficacy.
The result is that tryptophan pills are available only as dietary supplements, and it is unclear exactly what the correct dose might be. Since dietary supplements are not monitored for quality or contamination, it is difficult to tell which ones might be safe. Anyone who develops symptoms reminiscent of EMS while taking a tryptophan supplement should contact their healthcare provider right away.
Fortunately for us, tryptophan is also found in food. Have you ever wondered why grandparents used to suggest a glass of warm milk before bed? Milk is high in tryptophan. To enhance its effect in the brain, though, it needs to be taken with some extra carbs: sugar or starch. We don’t often recommend carb-loading, but one of our favorite insomnia “formulas” is a bowl of Cheerios with milk and honey. Other simple carbs (cookies, muffins, etc.) may work as well. (There’s even a company, Insomnia Cookies, that’s capitalized on this trick!) Try experimenting to find your favorite. We don’t recommend this approach for people with blood sugar problems, though.
5-HTP
Another option is 5-hydroxytryptophan (5-HTP). The body makes it from tryptophan and it can be taken as a supplement. It may help promote sleep, though research in humans is limited. There is animal research showing that a mixture of 5-HTP and GABA (gamma-aminobutyric acid) brings sleep on more quickly and leads to better quality sleep (Behavioural Brain Research, Sep. 1, 2016). A small study in 18 individuals got similar results from the combination of GABA and 5-HTP (American Journal of Therapeutics, Mar-Apr., 2010). Most 5-HTP supplements are derived from seeds of the plant Griffonia simplicifolia.
Melatonin
The rationale behind taking either tryptophan or 5-HTP is to encourage the brain to make more melatonin, a natural substance manufactured by the pineal gland deep within the brain. This compound is important for many reasons, including regulation of the body’s internal clock. Melatonin levels rise during darkness and are suppressed by strong light.
As we age, melatonin levels drop, and that may help explain why older people tend to have more sleeping problems. Researchers have studied the effect of giving melatonin to people with insomnia, shift workers and travelers who suffer jet lag. These studies have produced mixed results. Some show that it helps people fall asleep more quickly and stay asleep longer, but one meta-review of clinical trials concluded that it’s not effective for most sleep disorders. (It does seem to benefit people suffering from “delayed sleep phase insomnia:” those who go to bed very late, around 3:00 or 4:00 a.m., and get up late.) On the other hand, plenty of people swear by melatonin, and researchers believe that, at least in the short term, it seems safe.
The optimal melatonin dose may be as little as 300 micrograms, or 0.3 milligrams. But it’s difficult to find this dose, so it may be necessary to cut 1 milligram tablets into smaller pieces. (More is certainly not necessarily better, and doctors don’t know enough about possible side effects or long-term consequences of large doses.) Take it 30 minutes before bed. Melatonin should not be taken with warfarin (Coumadin, Jantoven).
Even though melatonin regulates the sleep-wake cycle, animals are not the only organisms that make this fascinating compound. Plants also synthesize melatonin from tryptophan (Journal of Pineal Research, Nov., 2016). Consequently, some plants known to be rich in melatonin may also offer benefit for the sleep-deprived.
Tart Cherries to Help You Snooze?
Some data suggest that tart Montmorency cherry juice (or supplements) could actually help you catch some evening Zs. In a randomized, double-blind, placebo-controlled trial, people who drank tart cherry juice for a week had higher melatonin levels, stayed in bed longer, slept more, and had better sleep quality. (Howatson, et al, “Effect of tart cherry juice (Prunus cerasus) on melatonin levels and enhanced sleep quality,” Eur J Nutr. 2012 Dec;51(8):909-16.)
For those who appreciate this tangy red fruit, a bit of tart cherry juice concentrate mixed into water may have a desirable effect. Some companies, like CherryFlex (www. cherryflex.com), also offer tart cherries in pill form. Cherries may have the added benefit of helping some folks with joint pain.
Daylight and Sleep
There’s growing evidence that bright light during the day can help reset the body’s natural sleep cycle. Preliminary research suggests that roughly 30 minutes to an hour’s worth of sunlight can be beneficial.
For those whose problem is waking up too early in the morning, the light exposure should be later in the day. For those who have trouble falling asleep at night, light exposure should be in the morning. (To overcome jet lag when flying west, try to get some light during the middle of the day when you land at your destination. If you fly east and lose fewer than seven hours, try to soak up some rays early.)
Conversely, getting too much light during the evening hours may not only disrupt sleep but could be harmful to your health in other ways. Bright light at night can reduce blood levels of melatonin, and low levels of this hormone have been linked to cancers of the prostate, lung, stomach, and breast.
Keeping your bedroom very dark at night may also help you fall asleep more easily. If you have a clock with a bright face, turn it away from you. This will have the added benefit of preventing you from watching the minutes tick away, which can increase anxiety and stave off sleep. Make sure to put your phone in sleep mode, turn off other bright electronic devices, and consider an eye mask or blackout curtains.
Magnesium
We’ve been hearing from our readers for years that magnesium, important for bones, nerves, muscles and brain function, may also help combat insomnia when taken at bedtime. Those who suffer from restless leg syndrome might particularly benefit; RLS can wake you in the middle of the night when you’ve been sleeping sweetly. A recent pilot study tested 200 mg of magnesium citrate a night for eight weeks (Journal of Clinical Sleep Medicine, May 13, 2024). Researchers report that the dozen people in the study had fewer symptoms of restless leg syndrome as their serum magnesium levels rose. We hope there will be larger, placebo-controlled studies of this effect.
An older placebo-controlled trial of magnesium in older adults with insomnia compared 500 mg of the mineral to placebo for eight weeks (Journal of Research in Medical Sciences, Dec., 2012). Those taking magnesium fell asleep more quickly and reported sleeping more soundly.
One reader shared this story:
“I often read about people having trouble getting a good night’s sleep. Perhaps my story will help someone.
“My pharmacist recently told me to take my magnesium tablets at bedtime instead of with breakfast. What a shocker to find such a difference in falling asleep. I no longer need to take melatonin or Tylenol PM.”
The recommended dose ranges from 250 to 500 milligrams daily. It may cause diarrhea, so reduce the dose or divide it if you develop loose stools. It is not safe for those with poor kidney function.
Acupuncture and Acupressure
Acupuncture is another possible treatment for chronic insomnia. Although there are several studies, experts are waiting for more definitive research demonstrating that acupuncture is effective against sleep problems (Cochrane Database of Systematic Reviews, Sep. 12, 2012). Nonetheless, acupuncture conducted by a knowledgeable practitioner is safe and might well be helpful (Pain Management, online Aug. 13, 2016).
If there is not a qualified acupuncturist in your region, you might wish to try acupressure. Many of our readers have reported that applying pressure to the inner arm, three finger-widths from the wrist between the two tendons, helps them sleep better. This spot is known as the Inner Gate. (You can view a YouTube video demonstrating the spot, also known as neiguan, here.)
There are commercial acupressure products available, like those by EasyComforts or Sea Band. Or you can make your own by taping or rubber-banding a kidney bean to the spot on your inner wrist that’s sensitive to acupressure.
SpatialSleep Headband:
A device that delivers customized frequencies to each ear helps some people with chronic insomnia. This wearable technology takes the form of a headband. It connects via Bluetooth to a smartphone app that determines the appropriate frequencies. Hearing different frequencies in each ear encourages brain waves conducive to sleep. The technology has been tested and shown to help both for falling asleep and staying asleep. Better yet: no side effects! You can find out more at SpatialSleep.com.
Herbal Remedies for Sleep
For centuries, people have used herbs to relax and fall asleep. Go no further than the lovely story of Peter Rabbit by Beatrix Potter. Remember the remedy Mrs. Rabbit relied on for Peter? It was good old chamomile tea. People have used this herb for generations for its soothing properties and to calm indigestion. We can think of no better way to end a long day than with a cup of chamomile tea.
People with allergies, especially hay fever, may be sensitive to chamomile. Keep in mind that the herbs discussed here have not been studied to see if they are safe during pregnancy. Prudence would suggest avoiding them during that vulnerable time.

Valerian
Another herb that may be even more effective for insomniacs is valerian, (Valeriana officinalis) which has long been used as a mild sedative. It doesn’t work instantaneously, though. It seems to be most helpful when taken each night for at least two weeks 30 minutes to 2 hours before bedtime. The dose is 300 to 600 milligrams daily, or 2 to 3 grams of the dried root for tea, steeped for 10 to 15 minutes. (It has one drawback: its pungent odor, reminiscent of sweaty socks and stinky cheese.)
One study in patients with acute coronary syndrome found that combining acupressure with valerian oil provided significantly better sleep than sham acupressure to points a centimeter or so away from the real points (Journal of Traditional and Complementary Medicine, Jan. 31, 2015). The acupressure points used in this study included ear spirit gate, hand shenmen, glabella, Wind Pool and Gushing Spring rather than neiguan.
One study showed that valerian (600 mg/day) was equal to the sleeping pill oxazepam (10 mg) in treating insomnia (Current Neuropharmacology, May, 2014). More research is needed to confirm the benefit of valerian and determine the best way to use it.
A recent review of the medical literature on sleep aids for older adults concluded that valerian has a modest effect in helping people get to sleep more quickly, but that it may also lead to next-morning drowsiness or grogginess (Clinical Therapeutics, online Oct. 14, 2016). A study done specifically to test whether valerian impairs driving ability found no problem, however (Accident; Analysis and Prevention, July, 2016).
According to Tieraona Low Dog, MD, valerian is unexpectedly stimulating instead of soothing for certain individuals (Low Dog, Healthy at Home, National Geographic, 2014). If you find that valerian makes you feel more awake, choose a different herb to help you sleep.

Kava
Kava (Piper methysticum) appears to be fairly effective at treating insomnia, particularly for people with anxiety (Nutrition Journal, Oct. 7, 2010). There are reports linking kava to liver toxicity, however, so it should be taken only under the supervision of a physician.
Passionflower
Passionflower (Passiflora incarnata) has traditionally been considered a helpful herb against insomnia. Clinical trials have been promising, but more rigorous studies have been called for (Journal of Ethnopharmacology, Dec. 12, 2013). One study compared a combination of passionflower, hops and valerian to the sleeping pill zolpidem (Ambien). The herbal compound performed similarly to the zolpidem among 78 participants (Indian Journal of Pharmacology, Jan-Feb., 2013).

Lemon balm
Lemon balm (Melissa officinalis) is a plant in the mint family named for its lemony scent. It has long been used in Europe to help people relax so they can get to sleep.
A review of research on lemon balm finds that it can be quite useful in countering anxiety (Journal of Ethnopharmacology, July 21, 2016). A study conducted in mice found that a combination of lavender (Lavandula angustifolia) and lemon balm worked better than either herb alone and helped mice sleep longer (Research in Pharmaceutical Sciences, Nov-Dec., 2015). A preliminary trial that was neither blinded nor placebo-controlled found that a standardized extract of Melissa officinalis, Cryacos®, reduced anxiety and alleviated anxiety-associated insomnia (Medical Journal of Nutrition and Metabolism, Dec., 2014).
Lavender
Lavender (Lavandula angustifolia) has been used both in aromatherapy and in oral preparations to encourage sleep. Two separate studies have examined the use of lavender essential oil administered in an inhaler for hospitalized patients and found it beneficial for people in this highly stressful situation (Nursing in Critical Care, July 27, 2015; Complementary Therapies in Clinical Practice, Feb., 2016). A study in a groups of college students instituted sleep hygiene practices and lavender oil inhalation (Journal of Alternative and Complementary Medicine, July, 2015). The students who were exposed to lavender essential oil while sleeping reporting waking more refreshed than those who practiced good sleep hygiene without the essential oil.
In another study, 170 volunteers who were having sleep difficulties took either the preparation Silexan® or a placebo (European Neuropsychopharmacology, Nov., 2015). At the end of 10 weeks, the participants taking the Silexan scored significantly better on several standardized scales of anxiety and sleep.
One advantage of lavender as aromatherapy is that it is readily available. You could try putting a sachet under your pillow or spritzing your pillowcase with scented water.
Q. After years of poor sleep, I now rub lavender-scented lotion and a drop of lavender essential oil on my forearms before bed. I finally get a good night’s sleep without medications.
A. Lavender oil derived from the Mediterranean plants Lavandula angustifolia or Lavandula stoechas has had a reputation as a sedative or calming treatment ever since medieval times (Evidence-Based Complementary and Alternative Medicine, volume 2013, article ID 681304). A review of research showed an improvement in sleep quality among people exposed to the odor of lavender oil compared to a placebo aroma.

Ashawagandha
Ashwagandha (Withania somnifera) is an herb from the Ayurvedic medical tradition. Tieraona Low Dog, MD, recommends it for people who are “wired and tired” to help them turn off the interior monolog and drift into sleep. It has anti-inflammatory, anti-oxidant and anti-stress properties (Alternative Medicine Review, Aug. 2000).
A double-blind study with 64 participants demonstrated that two months of treatment with 600 mg of Ashwagandha root extract (two 300 mg capsules daily) reduced scores on stress assessment scales significantly more than placebo (Indian Journal of Psychological Medicine, July 2012). Blood levels of the stress hormone cortisol also dropped significantly.
Rat studies show that Ashwagandha can normalize the sleep-wake cycle in sleep-deprived animals (Indian Journal of Pharmaceutical Sciences, Nov., 2008). Using mice as study subjects, investigators in Japan identified the water-soluble compound in the plant’s leaves that induces sleep (PLoS One, Feb. 16, 2017).
Moreover, a pilot study suggests that this herb can improve attention, decision making and memory in people experiencing mild cognitive impairment (Journal of Dietary Supplements, Nov. 2, 2017). Pharmacologic studies in brain tissue reveal that compounds in this plant activate GABA receptors (specifically GABA p1), which may explain its ability to counter anxiety and promote sleep (Journal of Ethnopharmacology, Aug. 2, 2015).
The dose ranges from 750 to 1,250 mg/day, and most people tolerate it without significant side effects (Journal of Ayurveda and Integrative Medicine, July, 2012). Kulreet Chaudhary, MD, recommends 400 to 500 mg in the morning and another dose before supper, preferably before 6 pm (Chaudhary, The Prime, Harmony Books, 2016).
Some Ashwagandha Cautions:
Unfortunately, there does not appear to be a lot of research on side effects and interactions. However, ashwagandha may affect thyroid function (Journal of Ayurveda and Integrative Medicine, Oct-Dec. 2014). Some people have reported digestive distress, including nausea and diarrhea.
One reader shared this:
“With so many articles citing the health benefits of ashwagandha, I figured it was worth a try. It’s not that I feel stressed out, but I did read that that this supplement would inhibit cortisol production. That sounded like a good idea.
“I started taking the supplement as directed, one 300 mg pill a day in the morning before breakfast. All went well for a few weeks.
“Then one morning I noticed big rumblings in my stomach, followed by a horrible bout of diarrhea—very similar to colonoscopy prep. I didn’t connect it to the supplement, so I took it again the next day with the same results.
“I stopped the supplement and within a few days was back to normal. After a week, I gave it another try and experienced the same results again. It is clear my body and ashwagandha are not compatible.
“Is this a common occurrence? Can use of this supplement produce serious complications?”
Some scientific research supports its use for easing anxiety, arthritis, neurodegenerative and cardiovascular conditions (Journal of Ethnopharmacology, Jan. 10, 2021). Although some people experience digestive upset, most studies have not found significant problems (Complementary Therapies in Medicine, Dec. 15, 2020). That said, you are not the first person to report severe diarrhea as a side effect.
Read on for another testimonial comparable to yours.
“You have written about ashwagandha as a way to manage insomnia. People should be very cautious about trying this even though it’s been used for centuries.
“My husband took it for insomnia and stress, but after only one capsule he became very ill: bloating, upset stomach and diarrhea. It lasted for almost 24 hours, and he was miserable. Obviously, some people can have an extreme reaction to it.”
Other side effects include drowsiness or headache. In addition, one visitor to our website reported an alarming drop in blood pressure. There is also a published case report of a cardiovascular reaction (Journal of Dietary Supplements, July 4, 2018).
It also might interact with MAO inhibitors such as selegiline, phenelzine or tranylcypromine. It should not be taken with such drugs, as it might reduce their effect (Phytomedicine, Dec. 2000).
Scientists have found that ashwagandha may normalize hormone levels in people with subclinical hypothyroidism (Journal of Alternative and Complementary Medicine, March 2018). To be prudent, people with overactive thyroid glands might want to avoid ashwagandha.
A rare complication of this herb may be liver damage.
German doctors report in the American Journal of Gastroenterology, Oct. 1, 2021:
“We here present the case of a 40-year-old man who experienced acute liver injury after intake of Ashwagandha extract. He was included in our prospective study on potentially hepatotoxic drugs, which has been described in detail previously. The patient had no medical history, a normal body mass index, and no harmful alcohol consumption. He had been consuming Ashwagandha extract (500 mg) for more than a year before he switched to Ashwagandha Now (Ashwagandha 450 mg; Now Foods, Bloomingdale, IL). Twenty days later, he experienced pruritus and jaundice.
“Ashwagandha has been associated with liver injury in rare cases and is listed in the LiverTox database. The signature of Ashwagandha-induced liver injury is highly similar to the evolution in our patient with pronounced pruritus and jaundice 2-12 weeks after initiation and prolonged hyperbilirubinemia with peak total bilirubin levels weeks after drug discontinuation.”
Anyone with elevated liver enzymes or a diagnosis of liver disease should avoid ashwagandha. Any symptoms of itching, jaundice, digestive distress or fatigue should be checked out promptly!
Catnip
Catnip (Nepeta cataria or Nepeta menthoides) has a reputation as a sleep-inducing herb, but few studies have been published on this use. The research we found demonstrated that a catnip extract may be beneficial in treating anxiety and depression (Iranian Journal of Medical Sciences, May, 2016; Complementary Therapies in Medicine, June, 2016). Many Nepeta species appear to have antioxidant properties and some are being investigated for their anticancer activity.
Hops
Hops (Humulus lupulus) is an essential ingredient in beer, of course, but it also has quite a reputation as a sleep aid. Although some research supports this tradition, it is far from conclusive (Journal of Ethnopharmacology, March 28, 2008). It appears that a combination of valerian and hops can increase the time spent sleeping and the quality of sleep, as assessed by EEG (European Journal of Medical Research, May 26, 2008).
One group of Spanish researchers has investigated the sleep-inducing properties of a single glass of non-alcoholic beer with supper. They have found this means of providing hops can benefit healthy nurses working night shifts and stressed-out university students (PLoS One, online July 18, 2012; Acta Physiologica Hungarica, Sep., 2014). There have also been hints that hops may help ease hot flashes and night sweats, which would be a great help to women as they go through menopause (Journal of Menopausal Medicine, online Aug. 30, 2016).

Sage
Sage (Salvia officinalis) is another traditional European herb reputed to help people fall asleep more easily. Like some of the other herbs, it does not appear to have been studied extensively. We found a trial of a combination product including extracts of sage leaves and alfalfa (Medicago sativa) in treating night sweats in 30 menopausal women (Minerva Ginecologica, May, 1998). The Italian scientists reported that two thirds of the women had their night sweats disappear, without changes to their estrogen levels. Sage could be toxic in large doses for long periods, so moderation in its use is essential.
St. John’s wort
St. John’s wort (Hypericum perforatum) has been used successfully to ease mild depression. A review of studies showed that a combination of St. John’s wort and black cohosh (Cimicifuga racemosa) can help ease night sweats so menopausal women can get some sleep (Gynecological Endocrinology, Sep. 2012). Individually, these herbs were not significantly better than placebo. Research in mice shows that Hypericum affects the same brain chemicals that benzodiazepine drugs do (Phytotherapy Research, Nov., 2012).
St. John’s wort is not expected to have the same types of side effects as typical benzodiazepines such as alprazolam (Xanax) or diazepam (Valium). Hypericum does have side effects, however. It can cause digestive distress and it may make both the skin and the eyes vulnerable to damage by sunlight (Current Neuropharmacology, May, 2014). In addition, this herb has the potential to interact with many medications to make them less effective.

Medications and Insomnia
Oral Decongestants Can Cause Insomnia
- Actifed
- Advil Cold & Sinus
- Allerest PE
- Alka-Seltzer Plus Sinus
- Allergy or Cold formulas
- Claritin-D
- Contac Non-Drowsy
- Dimetapp Sinus
- Dristan Sinus Maximum Strength
- Tylenol Sinus
- Ornex
- No-Drowsiness Allerest
- No Drowsy Sinarest
- Novafed
- Sinus Excedrin
- Sudafed
- Tavist D
Insomnia can be brought on by many things: anxiety, depression, pain, stress, frustration, elation, and a whole host of other emotions. But one source of sleeping difficulties that is rarely mentioned is medication. A surprisingly large number of prescription and over-the-counter drugs can make it harder to fall asleep.
OTC Trouble
We’ve already mentioned caffeine (found in lots of OTC pain relievers). But who would think that a cold or cough remedy could keep you awake at night? Aren’t those supposed to help you rest and recover? And yet the oral decongestants that are found in a wide variety of OTC medications can cause nervousness, anxiety, restlessness, and yes, sleeplessness.
One ingredient to be particularly wary of is pseudoephedrine. It can be found in so many OTC products that making a comprehensive list of them would be a real challenge. They’re now often stored behind the pharmacy counter. (The authorities have made pseudoephedrine harder to access than it once was because it’s often one of the key ingredients in illegal drugs like crystal meth. Yet it is still available without a prescription.)
Even antihistamines can sometimes make sleeping difficult. Although such drugs normally make people drowsy, children and some adults can actually be stimulated by them. Instead of helping them sleep, cold or cough remedies could have them wired for hours.
Prescription for Insomnia
Prescription drugs can also be culprits. The list of potentially insomnia-causing medications you’ll find below is only partial. Physicians rarely mention insomnia as a potential side effect, and yet, as you can see, there are many medicines that can create a sleeping problem.
They include blood pressure pills, asthma medicine and drugs for heartburn, anxiety, depression or attention deficit disorder. If you think your insomnia is related to your medication, please let your doctor know. There may be alternatives that he or she could prescribe that are less likely to keep you tossing and turning into the night.
Some Drugs That May Cause Insomnia
*Not all drugs that can contribute to insomnia are listed.
| albuterol | flunisolide (Aerospan) | nifedipine |
| allopurinol | fluoxetine (Prozac, Sarafem) | olanzapine (Zyprexa) |
| amlodipine | glipizide (Glucotrol) | omeprazole |
| amlodipine + benazepril | goserelin (Zoladex) | paroxetine (Brisdelle, Paxil) |
| amoxicillin | guanfacine | phenelzine (Nardil) |
| armodafinil (Nuvigil) | indomethacin | phentermine (Adipex-P) |
| azithromycin | interferon alpha | piroxicam |
| benazepril | isosorbide mononitrate | pramipexole (Mirapex) |
| buspirone | ketorolac | pravastatin |
| carvedilol (Coreg) | lamotrigine (Lamictal) | prednisone |
| celecoxib (Celebrex) | leuprolide (Eligard, Lupron, Viadur) | pregabalin (Lyrica) |
| ciprofloxacin | levodopa + carbidopa (Rytary) | propranolol |
| citalopram (Celexa) | levofloxacin (Levaquin) | ranitidine |
| clomipramine | levothyroxine (Levothroid, Levoxyl, Synthroid) | risedronate (Actonel) |
| clonidine | lisdexamfetamine (Vyvanse) | risperidone (Risperdal) |
| clozapine | losartan (Cozaar) | selegiline (Eldepryl, EmSam, Zelapar) |
| cyclobenzaprine | medroxyprogesterone | sertraline (Zoloft) |
| dasatinib (Sprycel) | methocarbamol | simvastatin (Vytorin, Zocor) |
| desvenlafaxine (Pristiq) | methylphenidate (Ritalin) | sulindac |
| dexmethylphenidate | metoclopramide (Reglan) | tapentadol (Nucynta ER) |
| diclofenac (Cataflam, Voltaren) | metoprolol (Toprol) | timolol (Timoptic) |
| eletriptan (Relpax) | metronidazole | tramadol (ConZip, Rybid ODT, Ryzolt, Ultram) |
| escitalopram (Lexapro) | montelukast (Singulair) | varenicline (Chantix) |
| esomeprazole (Nexium) | nabumetone | venlafaxine (Effexor) |
| etodolac | naproxen (Aleve) | ziprasidone (Geodon) |
| famotidine (Pepcid) |
Sleeping Pills
| Benzodiazepines |
|---|
| Ativan (lorazepam) |
| Centrax (prazepam) |
| Dalmane (flurazepam) |
| Halcion (triazolam) |
| Klonopin (clonazepam) |
| Librium (chlordiazepoxide) |
| Paxipam (halazepam) |
| ProSom (estazolam) |
| Restoril (temazepam) |
| Serax (oxazepam) |
| Tranxene (chlorazepate) |
| Valium (diazepam) |
| Xanax (alprazolam) |
Benzo withdrawal: a reader’s story
“I’ve been taking clonazepam for 3 years now, along with Requip & Topamax, for severe restless legs syndrome. That combination worked so well that I finally had relief from the torture I’ve been going through for 30 years!
“I also take Prozac for anxiety and morphine ER and Percocet for spinal stenosis and ruptured discs in my neck and back.
“Four months ago, my doctor told me he wouldn’t write any more clonazepam prescriptions because new laws won’t permit me to have it and pain meds at the same time.
“But instead of weaning me off, he just cut me off! The withdrawal was excruciating! I couldn’t sleep, the RLS came back with a vengeance, I had panic attacks, it was TERRIBLE!”
There’s no such thing as a perfect sleeping pill, but that hasn’t stopped humanity from searching. For centuries, insomniacs were prescribed sleeping potions like tincture of opium or chloral hydrate. Barbiturates like amobarbital (Amytal), pentobarbital (Nembutal) and secobarbital (Seconal) became popular for a while, but cases of abuse and overdose led researchers to look for something safer.
Benzodiazepines
In the late 1960s, benzodiazepines hit pharmacy shelves. Doctors embraced these new drugs with great enthusiasm. Chlordiazepoxide (Librium) and diazepam (Valium) became household names for relieving anxiety or stress. Flurazepam (Dalmane) quickly rose to the position of most-prescribed sleeping pill. These medications were initially believed not to create the problems of dependence people had experienced with older sleep medicines like narcotics or barbiturates. Overdose was unlikely to be deadly, even in combination with alcohol.
Eventually, however, it became apparent that benzos had their own problems. Dalmane could produce a morning-after “hangover.” Because the drug lingered in the body for days, it was possible to experience a carry-over reaction that made driving dangerous. Some people became confused, dizzy, lightheaded, drowsy, or disoriented.
With shorter-acting benzos like alprazolam (Xanax), lorazepam (Ativan), oxazepam (Serax), and triazolam (Halcion), many physicians thought once again that sleeping pill problems had been solved. But fast-acting Halcion and Ativan had such short durations that they could actually wake people up at night as they began wearing off. Some folks on these drugs experience daytime anxiety or even panic. Other side effects include memory problems, hyper-excitability, confusion, depression, daytime drowsiness, nausea, incoordination, light-headedness, feelings of unreality, paranoia, nervousness, and withdrawal insomnia on the evenings after they were used.
Addiction has been a controversial complication. Doctors had initially assumed it wouldn’t be a problem. But gradually reports surfaced that some people experienced substantial discomfort upon suddenly discontinuing benzos.
Eventually the evidence became compelling that even therapeutic doses could create dependence. Some people have symptoms if they stop after just 1-2 months of treatment. Gradual withdrawal with medical supervision is essential. Perhaps even more troubling, benzos are now believed to raise the risk for eventual Alzheimer’s or dementia (BMJ, Sept.9, 2014).
Z Drugs
In recent decades, so-called Z drugs have risen to prominence, such as eszopiclone (Lunesta), zaleplon (Sonata) and zolpidem (Ambien).
Zolpidem (Ambien, Edluar, Intermezzo, Zolpimist)
Zolpidem helps people fall asleep quickly and it starts working very fast—often within minutes, so hop right into bed after taking it so that you don’t get dizzy or fall asleep in the shower. Immediate-release zolpidem doesn’t help people stay asleep, but there’s a controlled-release (CR) formulation. Effects of the CR may last into the next day for some, making them groggy and less alert. Intermezzo is used for middle of the night awakening.
Zolpidem is best absorbed on an empty stomach and should not be taken with SSRI antidepressants such as fluoxetine (Prozac) or sertraline (Zoloft).
Most people take generic zolpidem, as insurance companies generally won’t pay for brand-name drugs. Some of our readers have complained that some generic formulations don’t work as well, wake them up in the night, or even cause nightmares.
Both Ambien and zolpidem may also produce rebound insomnia if stopped abruptly. Other less common side effects could include nausea, diarrhea, dizziness, daytime drowsiness, fatigue, weakness, difficulty with coordination, amnesia, memory problems, dry mouth, or headache. One side effect that has not gotten much attention is reflux or serious heartburn. This can disrupt sleep. For more information on this unexpected adverse reaction, check out this link. As with other meds, we urge short-term use and caution.
It seems like deja vu; at first, doctors were thrilled with Ambien, which seemed safe and non-habit-forming. But as more people have taken it, stories have emerged of some serious potential problems.
Bizarre Nighttime Behavior
Some people taking zolpidem report strange “sleep eating” episodes; when they wake up, they find food wrappers and crumbs, but they have no memory of chowing down. Even more dangerous is sleep driving.
Here are some stories from visitors to our website:
C. describes a situation we have heard many times:
“I took my zolpidem as prescribed. Went to bed and woke up with my face in an airbag. I totalled my car and am dwelling with a DUI citation. I could have killed myself or someone else and I have absolutely no recollection. I believe my defense should be involuntary DUI, but I doubt I can get my lawyer to agree to fight for that .”
James avoided an accident thanks to family members:
“My wife informed me the next day that I, in the dead of winter, ripped my t-shirt to pieces, and, totally naked, told her I was going out for a drive. Thankfully my nephew and wife prevented me from my midnight drive. I remember nothing else of this incident. I have stopped taking that type of medication, but this story is still the source of humor at family gatherings.”
Joe had no memory of his accident:
“I got into my car after going to bed and drove into a parked car two blocks from my house. I then proceeded to get out, walk home and get back into bed. That is where the police found me.”
D. also had an amazing story to share:
“I got ready for bed around 10:00 pm last night, took Ambien and fell asleep. The next morning my dog woke me up to let him out. As I passed through the kitchen I realized I had been sleepwalking/driving that night.
“I found a doggie bag full of food from a restaurant in the trash, my car was scratched up, my front door was wide open. I don’t understand how I could drive to a restaurant, order food, eat the food, ask for a doggie bag and pay the check (that’s if I even paid for it).
“I called my doctor to change medications and let her know what happen. I must have been very hungry.”
This all points to an amnesiac effect. Older people on sleep meds are nearly 5 times as likely to experience forgetfulness or confusion, and side effects like dizziness or daytime drowsiness could cause falls.
As with benzos, researchers are starting to have concerns that long-term use of Ambien and other Z drugs may increase the odds of developing Alzheimer’s and dementia (Medicine, May, 2015).
Likewise, as with every class of sleeping pill that’s come before, concerns over Z drugs and dependency have also emerged.
Eszopiclone (Lunesta)
Lunesta works in a way that’s similar to Ambien (and Sonata), but it does appear to maintain effectiveness longer; one study indicated that it could be taken for up to 6 months without losing efficacy or producing dependence. It’s possible, though, that rebound insomnia could result when Lunesta is stopped.
Some other reported side effects include unpleasant taste and dry mouth, headache, next-day drowsiness, dizziness, next-day memory impairment (anterograde amnesia), and difficulty with coordination. Like Ambien, Lunesta may lead to memory problems (forgetting things that happen after the sleeping pill is taken, aka anterograde amnesia).
Lunesta can be dangerous if taken with alcohol or other sedatives. It should not be taken with clarithromyacin (Biaxin), itraconazole (Sporanox), or ritonavir (Norvir). Older people need a lower dose, and no one should take eszopiclone in combination with another sleep aid, whether it is the OTC doxylamine or the prescription drug suvorexant. The narcolepsy drug sodium oxybate (Xyrem) is completely contraindicated in combination with eszopiclone.
Zaleplon (Sonata)
Sonata works in a way that’s similar to Ambien and Lunesta. What makes it unique is that it’s very short-acting. Because it wears off quickly, it can be taken by someone who wakes up in the middle of the night and can’t get back to sleep. You have to make sure that you’ll be able to get at least another four hours of solid sleep—otherwise, the medication may linger in your system come morning. (This same precaution applies to Intermezzo.) But as a benefit, if Sonata is taken to help people fall asleep at bedtime, it’s less likely to cause grogginess or next-day drowsiness the way other medications can.
Side effects may include headache, stomachache, dry mouth, constipation, back pain, and occasional next-day drowsiness. It shouldn’t be taken with a heavy meal; absorption may be slowed and effectiveness reduced. Zaleplon can interact with alcohol, cimetidine (Tagamet), imipramine (Tofranil), rifampin (Rifadin) and thioridazine. Older people should take no more than 5 mg.
Other Sleeping Pills
Ramelteon (Rozerem)
Rozerem works differently from every other sleeping pill on the market. It helps people fall asleep by targeting melatonin receptors in their brains. As a result, there’s no risk of addiction, it’s not classified as a “controlled substance,” and there’s no limit on the length of time one can use it.
Sounds like a miracle drug, right? Unfortunately, just as some doubts have been raised about the efficacy of melatonin, Rozerem may be less helpful for insomnia than other medicines, especially in reducing nighttime awakenings or helping people fall back to sleep in the middle of the night.
We’re also concerned about a side effect of Rozerem: it lowers testosterone levels and increases the hormone prolactin, which may lead to reduced libido, infertility, and osteoporosis. Other side effects may include next-day drowsiness, dizziness, nausea, fatigue, and headache. It’s not safe for people with liver problems, and it shouldn’t be taken by anyone on fluconazole (Diflucan), fluvoxamine (Luvox) or ketoconazole (Nizoral). It hasn’t been determined whether it’s safe during pregnancy.
Ramelteon is best taken 30 minutes before bed and, like Sonata, without fatty foods.
Suvorexant (Belsomra)
One of the newer and pricier prescription sleeping pills on the market is Belsomra. The manufacturer introduced its marketing of this drug with a bizarre TV commercial that featured two furry animated word pets. One is cat-like, white and spells out “Sleep” while the other is a fuzzy dog-like critter that is gray and represents “Awake.” The commercial emphasized the unique action of Belsomra to help “turn down wake messages by targeting and inhibiting the action of orexin, a neurotransmitter that plays a central role in sending wake messages.”
So how good is this sleeping pill? Most people, including health professionals, believe that a medication that has been approved by the FDA is backed by strong scientific evidence of effectiveness. In the case of Belsomra we will let you be the judge.
For openers, the dose that the FDA approved is 10 mg; if that doesn’t work, the doctor can prescribe 20 mg per night. According to experts for Consumer Reports, the higher doses “helped people stay asleep 16 minutes longer and fall asleep about 6 minutes faster compared to placebo.” We don’t know about you, but we didn’t find those results that impressive, especially considering that a month’s supply of Belsomra could cost over $300.
The 10 mg dose that the FDA approved preferentially was, according to Consumer Reports, “only studied in 62 people, and it’s unclear whether it improves sleep.” Perhaps that is why the publication QuarterWatch (January, 2016) that tracks adverse drug reports from the FDA’s database discovered that the drug didn’t work very well to help people get a good night’s sleep. Over 40 percent of the complaints to the FDA reported “that the drug was ineffective.” Side effects included “disturbed sleep, including nightmares, hallucinations, sleep paralysis, and sleep walking.”
Sleep paralysis is particularly disturbing, since people may report the inability to speak or move in this state as they fall asleep or try to wake up. Many people report that they experience a morning “hangover” effect in which they feel spacey or drowsy.
Some people experience the opposite effect. The drug purportedly produced a stimulant reaction leading to irritability, agitation or nervousness. There is an FDA warning about worsening depression or suicidal thoughts. The bottom line on Belsomra: We are not impressed by this sleeping pill, though the price will take your breath away at nearly $10 per pill. Consumer Reports suggests that if you need a prescription sleeping pill for a short term period (grief, stress, jet lag, etc), zolpidem (generic Ambien) might be the best choice. Just try not to get into an Ambien habit.
Trazodone (Oleptro)
For reasons that mystify us, one of the most commonly prescribed drugs for insomnia is trazodone (Oleptro). It was first approved by the FDA in 1981 for depression and has never been approved for insomnia. Nevertheless, many health professionals prescribe it off-label to people who have a hard time sleeping especially if they also seem depressed.
Side effects include morning “hangover” (next-day drowsiness), sedation, fuzzy brain, dry mouth, constipation, nausea or vomiting and blurred vision. Dizziness, unsteadiness and confusion may be especially problematic for older people. Trazodone can contribute to heart rhythm irregularities, and consequently it is contraindicated for anyone taking dronedarone (Multaq).
Dependency and Withdrawal
Benzo withdrawal: a reader’s story
“I’ve been taking clonazepam for 3 years now, along with Requip & Topamax, for severe restless legs syndrome. That combination worked so well that I finally had relief from the torture I’ve been going through for 30 years!
“I also take Prozac for anxiety and morphine ER and Percocet for spinal stenosis and ruptured discs in my neck and back.
“Four months ago, my doctor told me he wouldn’t write any more clonazepam prescriptions because new laws won’t permit me to have it and pain meds at the same time.
“But instead of weaning me off, he just cut me off! The withdrawal was excruciating! I couldn’t sleep, the RLS came back with a vengeance, I had panic attacks, it was TERRIBLE!”
If you think you may have developed a dependency on a prescription sleeping pill, seek the guidance of your physician in working out a plan for withdrawal. It could take several weeks or even more to comfortably get yourself off of the medication, but once you have, you may be able to use less habit-forming methods for satisfying sleep.
No one should ever stop taking prescribed medications without careful medical supervision. This is especially true if these medicines have been taken for more than a few weeks or months.
We’re by no means opposed to sleeping pills. They can be very helpful for handling occasional sleeping problems. The trick is not to get sucked into the vicious pill cycle: relying every night on drugs for sleep, then experiencing rebound insomnia when you try to cut back.
Experts recommend taking the lowest possible dose for the shortest period of time: a few days or up to a week or two. That should allow most people to avoid dependence.
Symptoms that may occur when getting off of benzodiazepine sleep meds:
- Anxiety, jitteriness
- Irritability, restlessness
- Agitation, panic
- Insomnia
- Derealization
- Tremor, twitching
- Difficulty concentrating
- Impaired memory
- Depression, vertigo
- Dry mouth, headache
- Nausea, GI upset
- Muscle pains, aches
- Sweating, shakiness
- Sensitivity to sound, light
- Paranoid reactions •
- Hallucinations, seizures
Over-the-Counter Sleep Medicine
Anticholinergic Drugs:
- Amitriptyline
- Atropine
- Benztropine
- Chlorpheniramine
- Chlorpromazine
- Clomipramine
- Clozapine
- Cyclobenzaprine
- Cyproheptadine
- Desipramine
- Dexchlorpheniramine
- Dicyclomine
- Diphenhydramine
- Doxepin
- Doxylamine
- Fesoterodine
- Hydroxyzine
- Hyoscyamine
- Imipramine
- Meclizine
- Nortriptyline
- Olanzapine
- Orphenadrine
- Oxybutynin
- Paroxetine
- Perphenazine
- Prochlorperazine
- Promethazine
- Protriptyline
- Pseudoephedrine
- Scopolamine
- Thioridazine
- Tolterodine
- Trifluoperazine
- Trimipramine
OTC medications are popular. One of the most common adverse reactions associated with antihistamines is drowsiness. People who take drugs like diphenhydramine (Benadryl) or doxylamine (Unisom) often complain of feeling sleepy and sluggish. Drug companies have turned this into a hugely successful marketing opportunity.
Diphenhydramine (DPH) is the main ingredient in many OTC sleeping pills, such as Advil PM, Aleve PM, Bayer PM, Excedrin PM, Nytol, Simply Sleep, Sominex, Tylenol PM and others. Check the labels of OTC sleep aids to see the active ingredient.
The Food and Drug Administration considers DPH safe and effective for insomnia, but many researchers have grown alarmed about its possible long-term risks, especially the possibility of dementia. In March 2015, JAMA Internal Medicine published research raising concerns about the effects of anticholinergic drugs on the brain over time. In the conclusion of this study, the authors wrote:
“Higher cumulative anticholinergic use is associated with an increased risk for dementia.”
Anticholinergic drugs such as doxylamine or DPH are also associated with some possible short-term side effects, such as confusion, cognitive impairment, dizziness, urinary retention, dry mouth, and visual disturbances. These can be particularly troubling side effects for older people, who may also be especially susceptible to next-day drowsiness or fuzziness. Other anticholinergic drugs are listed in the sidebar, although the list is not complete.
Sleep Apnea
Sleeping problems may sometimes be due to a condition called sleep apnea. When people with sleep apnea are asleep, their air passages get blocked, often for a few seconds at a time. They’ll actually stop breathing, sometimes many times a night. It can be caused just by the way a person’s neck or throat are formed, although obesity is also a risk factor.
Sufferers are often unaware of what’s happening, although they may not feel rested when they wake. Daytime tiredness and nighttime snoring are often symptoms of sleep apnea and should prompt a diagnostic work-up. Most people are not aware of their own snoring, so if you are wakened by a bed partner or a housemate snoring loudly, let the person know. They should be evaluated for sleep apnea.
Why Is Sleep Apnea a Problem?
This can be a serious condition if left untreated, raising the risks of high blood pressure, heart or liver problems and type 2 diabetes. People with sleep apnea are at increased risk for arrhythmias, especially atrial fibrillation (International Journal of Cardiology, Nov. 9, 2016; Journal of Atrial Fibrillation, April-May, 2016). Alcohol, pain relievers and sleeping pills may exacerbate sleep apnea.
How Is Sleep Apnea Treated?
Fortunately, there are several treatments. The most common is a CPAP machine that goes over the nose and mouth during sleep to provide continuous positive airway pressure. This prevents the breathing disruptions and also reduces the likelihood of complications such as an arrhythmia.
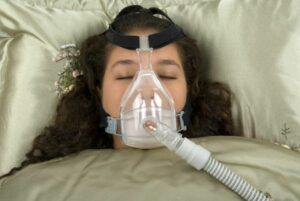
Some people with sleep apnea may also be able to use a less invasive oral appliance, adjustable and custom-made, that moves the lower jaw forward a bit during sleep. Finally, some people benefit from a fairly minor surgical procedure.
If you suspect that you or a partner has sleep apnea, it’s crucial to talk to your doctor, not just for your sleep, but for your overall health.
Cognitive Behavioral Therapy for Insomnia
If insomnia is an ongoing problem it can be very useful to consult a sleep specialist. Many use a method called cognitive-behavioral therapy (CBT), which has been shown to be quite helpful for managing insomnia. Nearly all will give you guidelines on “sleep hygiene,” how to change your habits, etc.
It is even possible to learn effective cognitive-behavioral therapy online. A study recently published in JAMA Psychiatry (Nov. 30, 2016) included 303 insomniac volunteers. They were randomly assigned to online sleep education (the control group) or to participate in a 6-week online CBT program called SHUTi (for Sleep Healthy Using The internet). Participants filled out questionnaires rating their sleep symptoms at the start of the study, after nine weeks, and after one year. The CBT program reduced the time it took them to fall asleep and decreased the amount of middle-of-the-night waking. More than half (56.6%) no longer qualified as having insomnia after the intervention. An editorial published in the same issue remarks, “On the whole, the findings suggest that SHUTi is a promising treatment for patients with insomnia.” They foresee a time when people might seek out a specialist for help with sleep problems only if an internet-based CBT program failed.
If you’d like to visit a sleep lab or specialist in person, you can visit the website of the American Academy of Sleep Medicine (www.sleepeducation.org/find-a-facility). They have a database of sleep centers and can help with a referral.
Recommended Health Guides
Dealing with Depression
This guide discusses the signs and symptoms of depression, which may often include sleep disruption. Download it to learn about drug and nondrug treatments.
Get advice on how to discontinue drugs like Cymbalta, Effexor or Paxil that can trigger unpleasant or intolerable withdrawal symptoms if they are stopped suddenly.
Digestive Disorders
Download this guide to learn about controlling nighttime heartburn that may be keeping you awake.
Drug and Alcohol Interactions
Most sleeping pills are incompatible with alcohol. You can download this guide to learn about the interactions that could pose problems.
Leg Pain
This guide discusses nighttime leg cramps and restless legs syndrome. Download it for more information on these sleep-wreckers.
Alternatives for Arthritis
If arthritis pain is keeping you awake at night, you can download this guide to learn about home remedies that may ease the discomfort.
Colds, Coughs & the Flu
When you are miserable with a cold and a cough is keeping you awake, download this guide to learn how you can soothe the cough and get a good night’s sleep.
Menopause
Download this guide to learn what can be done for hot flashes and night sweats.
Publication Information
Published on: November 26, 2024
|
Last Updated: April 16, 2026
Publisher: The People's Pharmacy
© 2026 The People's Pharmacy
