Do you have high blood pressure? There’s a 50% chance that you do. That’s because anything above 120/80 is now considered hypertension. But was your blood pressure measured correctly? It is astonishing how many mistakes are made during what seems like such a simple procedure. A study published in the journal Hypertension (Sept. 5, 2024) suggests that most home blood pressure monitors come with an arm cuff that could be too small for many people. That will overestimate blood pressure readings, which could lead to unnecessary medications. It’s not just home monitors, though. We have heard from a great many people who report serious errors when blood pressure is measured in a clinic or doctor’s office.
When Was Your Blood Pressure Measured?
We are big fans of home blood pressure measurement. That’s because there is no such thing as a single BP reading. If you are driving to work and suddenly see a blue flashing light in your rear view mirror, your blood pressure will likely skyrocket. That’s because you may have exceeded the speed limit or violated some other traffic law and are about to be pulled over. If you are hiking in the woods and see a copperhead snake directly in front of you, chances are good that your BP will also rise pretty fast.
But if you are relaxing with your feet up and are reading a good book or watching a delightful comedy on television, your BP may be lower than normal. Trying to decide what is your “normal” blood pressure requires regular measurements under a variety of conditions. That’s why a single BP reading in a doctor’s office is not very reliable.
Does Your BP Device Have the Right Sized Cuff?
The study published in Hypertension (Sept. 5, 2024) points out a serious flaw with home blood pressure measurements. It was titled:
“Arm Size Coverage of Popular Over-the-Counter Blood Pressure Devices and Implications in US Adults”
This study was carried out by the Johns Hopkins Bloomberg School of Public Health. It identified a flaw in home blood pressure measurements. The default cuff size that comes with most home blood pressure monitors can be too small. Of the 10 devices that were reviewed, 9 offered cuff sizes that ranged from 22 to 42 cm in circumference. Data from the National Health and Nutrition Examination survey reveals that over 17 million adults have an arm circumference that is either smaller than 22 cm or greater than 42 cm. (To calculate or measure your cuff size, 1 inch equals 2.54 cm).
A blood pressure cuff that is too small for a large arm can overestimate blood pressure readings by 5 to 10 mm of mercury. Equally, a cuff that is too large can underestimate blood pressure readings by the same amount. A 10 point error is enough to change a diagnosis from normal to hypertensive.
The authors of the research point out that:
“Hypertension is the leading cause of cardiovascular disease and premature death worldwide. An accurate blood pressure (BP) measurement is essential for the diagnosis and treatment of hypertension; however, crucial steps to obtain accurate measurements (eg, patient positioning) are often not fully taken due to time and resource constraints.”
More about how doctors, nurses and health technicians take blood pressure shortly.
Here is the bottom line on the research:
“Our study found that, based on the standard cuff size provided, most of the popular devices in a larger online retailer accommodate an arm circumference of 22 to 42 cm. This indicates that 6.7% of US adults are not eligible to use these devices as is. While seemingly a small proportion of the population, this corresponds to ≈17 million adults in the United States.”
Let’s be perfectly honest. A lot of Americans have big arms. Some men work out and build up large, muscular biceps. Other folks are on the heavy side when it comes to weight. The result is an arm that is larger in circumference than 42 cm (16.5 inches).
Some older women have small arms (less than 22 cm or 8.6 inches). That will also lead to incorrect measurements. The idea that 9 out of 10 of the devices monitored by the researchers would not accommodate someone with a smaller or larger arm circumference is disappointing.
The lead author, Kunihiro Matsushita, MD, PhD, is quoted:
“The fact that millions of Americans are affected shows that this is not a small problem; and probably the easiest solution is for retailers just to offer a wider range of cuff sizes for no extra cost.
“Consumers should be able to buy the blood pressure cuff sizes they need just as they can buy clothing sizes they need.”
The bottom line is that people with nonstandard-sized arms should make sure to purchase blood pressure cuffs of the correct size. When blood pressure is measured in a health care setting, the nurse or technician should also make sure to use the correct-sized cuff!
How Was Your Blood Pressure Measured in a Health Care Setting?
Let’s start with the most basic question: who took your blood pressure measurement? If we climbed into a time machine and set the clock for 1980, the doctor or nurse probably measured your blood pressure with a sphygmomanometer and a stethoscope. They would listen to the sounds over the brachial artery in the crook of your elbow.
The first “whoosh” of blood equals systolic blood pressure and the last “whisper” represents diastolic blood pressure. These “Korotkoff” sounds correspond to the peak pressure at the moment the heart contracts (systole) and pumps blood through arteries and the lowest blood pressure when the heart relaxes (diastole).
Medical students and nursing students were taught the correct technique early in their education. This was considered a crucial skill.
From Manual to Automated BP Measurements:
Then along came automated blood pressure devices. It was no longer necessary to use a stethoscope to listen for the Korotkoff sounds. The electronic devices became highly accurate at picking up the faint whooshing sounds. Doctors and nurses still did the measurements, though, and mostly followed the correct procedures to verify accurate readings.
These days it is rare for these health professionals to spend valuable time measuring blood pressure. This task is generally left up to certified medical assistants (CMAs). A medical assistant’s hourly salary can range from about $12/hr to around $16/hr. That means the annual salary runs from about $24,000 to around $35,000, depending upon the state and the years of experience.
Nurses, on the other hand, average anywhere from about $37/hr to $44/hr. And annual salaries for an RN can range from around $45,000 to about $83,000. Some places pay more. The annual salary of a nurse in Sacramento, California is $108,000 whereas the annual salary of a nurse in Pascagoula, Mississippi is around $89,000. Needless to say, the education and compensation of an RN is quite different from a CMA.
We mention education and salary only because we have seen first hand how medical assistants can make a lot of mistakes when measuring blood pressure.
Was Your Blood Pressure Measured With the Right-Sized Cuff?
Have you ever had a medical assistant measure your arm circumference? We would be surprised if you said yes. But the size of the BP cuff is really important! An article in the American Journal of Hypertension (June, 2022) notes that:
“As the world-wide prevalence of obesity continues to rise, the importance of screening, diagnosing, and treating hypertension to recommended targets cannot be overstated. Unfortunately, in the setting of obesity, the accurate measurement of blood pressure (BP) is more difficult, primarily related to inadequate cuff size and fit. Most standard BP cuffs currently in use are designed for cylindrical arms and are rectangular in shape. When these cuffs are applied to individuals with obesity, they are often too long on the arm, with the lower cuff border covering the antecubital fossa, and too loose at the distal end of the cuff, leaving substantial space between the skin and the interior of the cuff. This poor cuff fit leads to nonuniform compression of the brachial artery with significant implications for BP measurement accuracy.”
If the Cuff is Too Small, There is Another Problem: Pain!
We recently heard from a reader of our syndicated newspaper column:
Q. When the assistant in the doctor’s office takes my blood pressure, it hurts. In fact, I have wondered if the pain in itself makes my BP skyrocket. They pump it up again, and it still hurts really, really badly. Does anybody else have this problem?
A. Pain can raise blood pressure. Unfortunately, your experience is not rare.
Another reader reports:
“The new automatic BP cuffs at the doctors’ office hurt like heck. Suddenly they said I had hypertension and put me on a medication that made me cough.
“I quit that med. When I was at the office several months later, I insisted on manual BP readings. I was not surprised that my BP was back to its usual 116/70. Apparently, pain does raise your BP!”
Blood pressure cuffs come in different sizes. The wrong cuff could cause pain. You should also get time to relax before a BP reading. Your arm should be supported at heart level. Never talk while your blood pressure is being taken.
Lowering the Blood Pressure Bar:
If you had your blood pressure measured 30 years ago and it was 145/95, your chart would probably say you had “mild” or “borderline” hypertension. You might have been told to lose weight, cut back on salt or exercise more.
In 2017 the same reading would be interpreted quite differently. More specifically, you would be diagnosed with stage 2 hypertension. That year the American College of Cardiology and the American Heart Association (AHA) determined that hypertension was anything over 130/80 (Annals of Internal Medicine, March 6, 2018).
Previous guidelines urged doctors to treat patients whose blood pressure measured 140/90 or higher. The first and higher number is systolic blood pressure: the pressure within the vascular system when the heart is squeezing blood through it. The second number, diastolic blood pressure, is the pressure remaining while the heart relaxes between beats. Under the new criteria, blood pressure at or above 130/80 is defined as high blood pressure. Most people at that measurement will need to take steps to reduce it.
Why the Change In Defining High Blood Pressure?
The lower threshold appears to flow from a study called SPRINT that was published two years ago. It showed clearly that people who were able to lower their systolic blood pressure close to 120 were 25 percent less likely to have a heart attack or a stroke. In absolute terms, the difference did not look enormous: 1.65 percent of those getting systolic blood pressure down near 120 had a cardiovascular complication compared to 2.19 percent of those whose systolic blood pressure was lowered only to 140. Still, when you consider how many millions of us (approximately 103 million) have blood pressure at or above 130/80, a little difference can add up to an awful lot of people. Avoiding a heart attack or stroke will be a huge benefit for them.
Roughly half of all adults in America (over 100 million people) were instantly labeled hypertensive. Even though their American colleagues were lowering the bar, European cardiologists retained the 140/90 cutoff (Circulation Research, March 2019).
Do You Have High Blood Pressure?
If you live in the U.S., you now have high blood pressure if your readings are greater than 120/80. “Normal” blood pressure is defined as anything less than 120/80. That’s true whether you are 25 or 85. If you can’t get your blood pressure below that cutoff with weight loss, exercise or a low-salt diet, many doctors feel obligated to prescribe medications. It is possible to lower blood pressure without drugs, but it requires diligence and effort: exercise, meditation and a DASH diet with plenty of vegetables and fruits can work.
Blood Pressure Measured Correctly:
We have not made up the following recommendations. They come from the American Heart Association (AHA)(Hypertension, May, 2019)
- You should always empty your bladder prior to blood pressure measurement. If you had to deal with traffic congestion, parking problems or any other stressors, you should be given time to go to the bathroom and then recover your equilibrium.
- When it comes time to have your blood pressure taken, you should be given more time to sit quietly (for at least five minutes) in a comfortable chair prior to any measurement. Feet should be flat on the floor and the back must be supported. The temperature in the room should be at least 72 degrees F. Blood pressure should never be measured while the patient sits on an exam table with feet and arms dangling.
- Most important, the blood pressure cuff should be the right size for your arm, neither too big nor too small. The arm must be supported at heart height.
- Equally important, there should be no talking during blood pressure measurement. Even casual conversation can artificially raise blood pressure.
- Multiple readings are appropriate with at least a minute between each reading. The AHA recommends three measurements. You should not be told you are hypertensive based on one reading!
Readers Sound Off About Bad BP Measurements:
Readers frequently complain about faulty blood pressure technique. One woman reported that having her blood pressure measured is like being pinched really hard.
She asks:
“If pain can elevate BP during other procedures, why not if someone is squeezing the daylights out of my arm?”
The answer is yes, pain can raise blood pressure (Journal of Clinical Hypertension, Aug. 2013). The cuff is likely the wrong size. The authors of this paper note:
“Another widely used stimulus has been the forearm ischemia [reduced blood flow] produced by a cuff inflated to cut off the blood supply. In this test, the degree of pain correlates with the increase in BP and vascular resistances.”
No one should be subjected to pain while having their blood pressure measured!
Another reader asks:
“I have seen techs, nurses, and doctors place the blood pressure cuff over heavy sweatshirts and take a blood pressure. When I asked about this, they all said it did not matter. Does it?”
Answer: yes. The article in the journal Hypertension that describes the AHA’s recommendations about proper blood pressure techniques states:
“Remove clothing covering the location of cuff placement.”
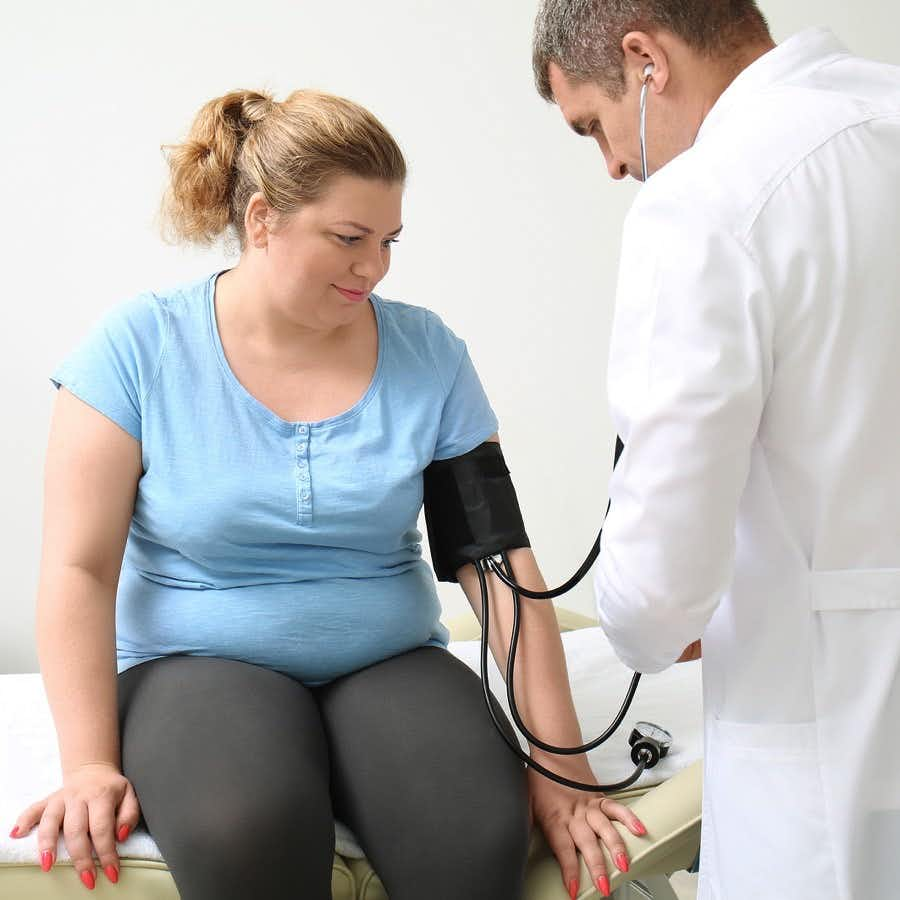
By the way, take a look at the photo at the top of this article. How many mistakes did you count? Here are some hints:
- Is the patient sitting in a comfortable chair?
- Is her back supported?
- Does the patient have her feet resting on the floor?
- Is the patient’s arm supported at heart height?
- Is the blood pressure cuff the right size?
Answers: No, No, No, No, No!
Joan asks a very reasonable question:
“Rather than a picture showing the wrong way to take blood pressure, perhaps a photo to show the right way.”
Here is an example of proper technique:

Close-up Of Doctor’s Hand Measuring Blood Pressure Of Male Patient
Please note that the patient’s arm is supported at heart level! The shirt has been removed so that the cuff is directly on the skin. The cuff is the correct size for this arm. The doctor is using an old-fashioned stethoscope and is applying it directly over the brachial artery. The man is sitting in a chair with his feet and back supported. Take a second to scroll up to the top of the page to see the difference between this BP measurement and the woman sitting on the exam table.
How Can You Tell If You Have High Blood Pressure?
Because so many mistakes can be made in a doctor’s office or hospital clinic, we encourage people to measure their own blood pressure at home. Our eGuide to Blood Pressure Treatment provides guidelines and strategies for both measurement and management of hypertension. It is available in the Health eGuide section.
You may also want to listen to our podcast: Show 1134: Can you Control Your Blood Pressure Without Drugs?
Citations
- Carey, R. M., et al, “Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults: Synopsis of the 2017 American College of Cardiology/American Heart Association Hypertension Guideline,” Annals of Internal Medicine, March 6, 2018, DOI: 10.7326/M17-3203
- Muntner, P., et al, “Measurement of Blood Pressure in Humans: A Scientific Statement From the American Heart Association” Hypertension, May, 2019, https://doi.org/10.1161/HYP.0000000000000087
- Taler, S.J. and Brady, T.M., "The Challenge of Accurate Blood Pressure Measurement: Optimizing Cuff Size and Fit Is Important for All, Not Just for Some," American Journal of Hypertension, June 16, 2022, doi: 10.1093/ajh/hpac026
- Kaur, E., et al, "Arm Size Coverage of Popular Over-the-Counter Blood Pressure Devices and Implications in US Adults," Hypertension, Sept. 5, 2024, https://doi.org/10.1161/HYPERTENSIONAHA.124.23473