Doctors appreciate ACE (angiotensin receptor enzyme) inhibitors for lowering high blood pressure. They have been first-line treatments for hypertension for many years. We used to think drugs such as benazepril, captopril, enalapril, fosinopril and lisinopril were “remarkable.” That was before we heard from hundreds of patients that an ACE inhibitor cough could be devastating. Now, we are also reading about the possibility there is a link between drugs like lisinopril and lung cancer.
Our Historical Perspective on ACE Inhibitors:
In our book, Best Choices from the People’s Pharmacy (2006), we were enthusiastic about ACE inhibitors. Here is how we described such drugs:
An ACE Up Your Sleeve
“One of the most extraordinary advances in pharmaceutical research and blood pressure management evolved out of the jungles of Brazil. A Brazilian scientist noted that when people were bitten by the poisonous jararaca snake, they experienced a dramatic drop in blood pressure. By harnessing the power of the snake venom to lower blood pressure, pharmacologists were able to isolate chemicals that could be used as drugs.
“These venom-derived compounds block an enzyme that converts a naturally occurring chemical called angiotensin I into a powerful vasoconstrictor called angiotensin II, which in turn raises blood pressure. The drugs are called angiotensin-converting enzyme (ACE) inhibitors. The first was captopril (Capoten), and it was followed by a wide range of other chemicals that have revolutionized the treatment of high blood pressure.
“By all accounts, ACE inhibitors are now considered to be the best choices in the treatment of high blood pressure for many patients.”
ACE Inhibitors vs. ARBs (angiotensin receptor blockers):
ARBs have a somewhat similar mechanism of action. They work by impeding the vasoconstrictor activity of angiotensin II. Read more about this intriguing class of medications at this link.
Over the last year and a half, ARBs like losartan, valsartan and irbesartan have been under a nitrosamine contamination cloud. There have been so many recalls of these drugs that we long ago lost count. We suspect that many physicians have turned to ACE inhibitors to avoid questions about quality.
A New Concern: ACEIs like Lisinopril and Lung Cancer?
This reader describes the new dilemma:
Q. My mother took lisinopril for years to control her blood pressure. She regularly went to her physician complaining of a chronic cough, but he kept telling her it was allergies and prescribed Zyrtec.
After a year of this, her doctor decided she must have GERD and sent her to a gastroenterologist. The specialist found nothing.
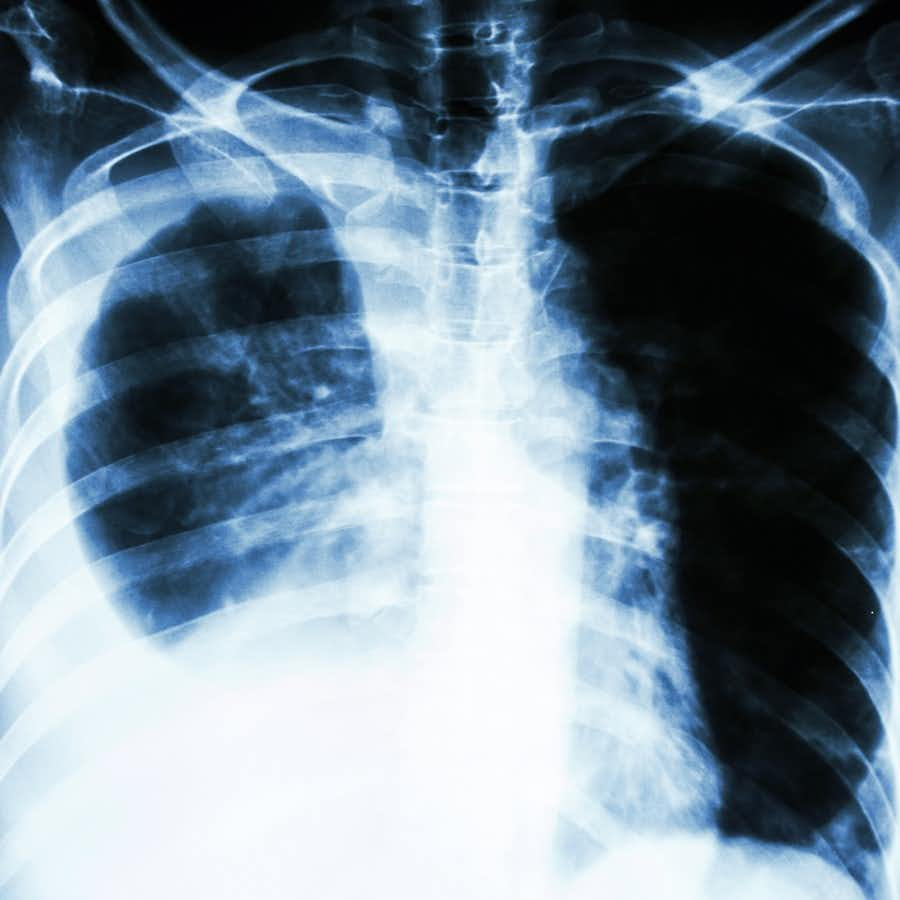
Not once did anyone prescribe a chest X-ray. When she started losing weight and feeling extremely fatigued, I insisted on a chest X-ray. They found advanced lung cancer and she died six months later. Is there a link between lisinopril and lung cancer?
A. Lisinopril is one of the most frequently prescribed medications in the U.S. It is an ACE (angiotensin converting enzyme) inhibitor. More than 20 million Americans take this drug because it is so effective for blood pressure control.
For the most part, lisinopril is considered safe. It can cause a chronic cough, however. That is something your mother’s doctor should have considered. We have been puzzled why so many doctors apparently overlook this classic complication of ACE inhibitors.
Lisinopril and Lung Cancer?
Only a few studies have addressed your question about lisinopril and lung cancer. In 2012, Canadian researchers reviewed the medical records of more than a million individuals (PLOS One, Dec. 12, 2012). They found that long-term use of ACE inhibitors was linked to a modestly increased risk of lung cancer.
A more recent study also found a slightly higher rate of lung cancer among patients who had taken an ACE inhibitor for at least five years (BMJ, Oct. 24, 2018).
Here is what the authors conclude:
“In this large population based study of nearly one million patients, the use of ACEIs was associated with an overall 14% increased risk of lung cancer. Associations were evident after five years of use and increased with longer durations of use, particularly among patients who used ACEIs for more than 10 years (31% increased risk). Although the magnitudes of the observed associations are modest, ACEIs are one of the most widely prescribed drug classes; in the UK, 70.1 million antihypertensives are dispensed each year, of which approximately 32% are ACEIs. Thus, small relative effects could translate into large absolute numbers of patients at risk for lung cancer.”
The authors call for more research that would involve patients “exposed for longer durations.” The Food and Drug Administration rarely requires such long-term trials. As a result, any connection between lisinopril and lung cancer is not likely to be uncovered for a very long time, if ever.
It’s virtually impossible to determine whether any given case of cancer is the result of exposure to a medication. The FDA does not make this any easier. The agency reports that animal studies did not reveal any signs of a “tumorigenic effect” with lisinopril. But in the adverse events section of the official prescribing information for lisinopril the FDA lists rare, serious, possibly drug-related events reported in uncontrolled studies or marketing experience. Included in this very long list is “malignant lung neoplasms.”
What NOT to Do About the Question of Lisinopril and Lung Cancer:
We always emphasize that no one should ever stop any medication without discussing all concerns with the prescribing physician. That is especially true for a commonly prescribed drug for hypertension. Print the article from the BMJ and give your provider time to read and consider it. The absolute risk appears small, but given the number of people taking lisinopril and its cousins, the risk may not be trivial.
Readers can learn more about other alternatives for controlling hypertension in our Guide to Blood Pressure Treatment. It is available in the Health eGuides section of www.PeoplesPharmacy.com.
Share your own thoughts about ACE inhibitors in the comment section below.
Do you appreciate The People’s Pharmacy? We try to be your Drug Watchdog, keeping an eye on Big Pharma, the generic drug industry and the FDA. If this is important to you, please consider supporting our work by signing up for our ad-free option at this link. You can also make a one-time donation at this link. Many thanks!

