Blood Pressure Solutions
Table Of Contents
- High Blood Pressure
- White Coat Hypertension
- Home Monitors
- To Get An Accurate Reading
- Non-Drug Options
- Eat Drink and Be Merry
- Other Things to Avoid
- Diuretics
- ACE Inhibitors
- Angiotensin Receptor Blockers
- Aliskiren
- Calcium Channel Blockers
- Beta Blockers
- What Happens When Nothing Works Well?
- Endothelin-Receptor Antagonist:
- Final Words:
High Blood Pressure
You have no doubt heard high blood pressure referred to as the silent killer. That’s because most people cannot feel their blood pressure. They don’t know when it is elevated and they are unaware of the damage going on inside the body. Symptoms do not show up until health problems have progressed. Uncontrolled hypertension takes a toll on blood vessels. That in turn increases the risk of heart attcks, strokes and aneurysms. That’s when a weak spot in a blood vessel (like the aorta) bulges. If an aneurysm starts leaking blood or blows, it can be fatal. Other complications of hypertension include kidney disease, heart failure, eye damage and dementia.
Everyone agrees that getting hypertension under control reduces the likelihood of experiencing such catastrophes. But there is controversy about:
- When blood pressure should be considered a problem
- How best it should be treated
- The pros and cons of drug therapy
- Are there nondrug ways to help control hypertension?
You will be surprised to learn how much health professionals disagree about things like the proper measurement of blood pressure, who should be treated and when treatment should start or stop.
Do You Have High Blood Pressure?
There is a very good chance that you do. That’s because the latest guidelines from the the American Heart Association (AHA) and the American College of Cardiology (ACC) have lowered the diagnostic bar. The label “hypertensive” used to be reserved for people with systolic blood pressure (the upper number) over 150 and diastolic blood pressure (the lower number) above 99.
The ACC and the AHA have created guidelines for blood pressure:
Normal blood pressure is considered anything less than 120/80.
Elevated blood pressure is 120-129 systolic and over 80 diastolic.
Stage 1 hypertension is 130-139 systolic and/or 80-89 diastolic.
Stage 2 hypertension is over 140 systolic and at least 90 or greater diastolic.
You can read more about the ACC/AHA guidelines at this link.
You Probably Do Have Hypertension If You Accept the Guidelines:
If you have systolic blood pressure over 130 or diastolic blood pressure over 80 you are now defined as hypertensive. That means that roughly half of all adults in the United States (100 million people) have high blood pressure. It wasn’t always so.
Dr. Charles Friedberg was a prominent cardiologist during the mid 20th century. In his well regarded textbook of the day he wrote that mild benign hypertension (defined then as blood pressure up to 200/100) did not require treatment (Journal of Clinical Hypertension, Suppl. 8, Aug., 2006). Another highly regarded cardiologist of the day, Dr. W. Evans, considered blood pressure elevated when it was greater than 180/110. Given what we now know, such numbers were far too lenient.
During the 1960s and 1970s data collected from the Framingham Heart Study encouraged doctors to get blood pressure down from such high levels. Doing so could reduce a patient’s risk for stroke, heart failure and kidney damage. The first guideline was published by the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure in 1977. It recommended treatment if diastolic blood pressure (the second and lower number) reached 105.
By 2003, the official guideline was that hypertension started at a blood pressure of 140/90. Until August 15, 2012, if you asked almost any American physician whether someone with a blood pressure reading of 145/95 should be treated with medication, the answer would have been a resounding yes! Many doctors were moving in the direction of getting patients closer to 120/80.
The Cochrane Collaboration Controversy:
That became a bit more confusing after August 15, 2012, though. The idea that lower blood pressure is always better was challenged in a review by the Cochrane Collaboration. This organization represents the highest level of scientific scrutiny of available studies. The experts who analyze the data are independent and objective and have come to be regarded as the ultimate authority on the medical interventions they evaluate.
The Cochrane experts reviewed the medical literature on hypertension. They focused on four randomized controlled trails involving 9,000 patients. Their conclusions created controversy because they suggested that many Americans might be treated too aggressively.
Here is what the Cochrane Collaboration found:
“Individuals with mildly elevated blood pressures, but no previous cardiovascular events, make up the majority of those considered for and receiving antihypertensive therapy. The decision to treat this population has important consequences for both the patients (e.g. adverse drug effects, lifetime of drug therapy, cost of treatment, etc.) and any third party payer (e.g. high cost of drugs, physician services, laboratory tests, etc.). In this review, existing evidence comparing the health outcomes between treated and untreated individuals are summarized. Available data from the limited number of available trials and participants showed no difference between treated and untreated individuals in heart attack, stroke, and death.”
The abstract concluded:
“Antihypertensive drugs used in the treatment of adults (primary prevention) with mild hypertension (systolic BP 140-159 mmHg and/or diastolic BP 90-99 mmHg) have not been shown to reduce mortality or morbidity in RCTs [randomized controlled trials]. Treatment caused 9% of patients to discontinue treatment due to adverse effects. More RCTs are needed in this prevalent population to know whether the benefits of treatment exceed the harms.”
Whiplash from “SPRINT”
Let’s jump from August 2012 to September 2015. That is when the SPRINT (Systolic Blood Pressure Intervention Trial) study was terminated early because the results were so good. Patients with hypertension who got their systolic BP below 120 were less likely to have heart attacks or other cardiovascular events (New England Journal of Medicine, Nov. 26, 2015). You can read more details of the SPRINT study at this link.
At the annual meeting of the American Heart Association on November 13, 2017 new guidelines were introduced (Hypertension, June, 2018). Under the new criteria, blood pressure at or above 130/80 was defined as hypertension. Many blood pressure monitors will tell you that if your blood pressure is 132/80 you have Stage 1 hypertension. That can make some people quite anxious.
Blood pressure greater than 120/80 used to be considered prehypertension. After SPRINT, though, many doctors considered such patients “hypertensive” and began treating them aggressively to get BP readings below 120/80.
The SPRINT-MIND Mystery:
There was a follow up to the SPRINT trial.
The SPRINT-MIND study asked:
“Does intensive blood pressure control reduce the occurrence of dementia?”
It was published in JAMA (Feb. 12, 2019).
The answer:
“Among ambulatory adults with hypertension, treating to a systolic blood pressure goal of less than 120 mm Hg compared with a goal of less than 140 mm Hg did not result in a significant reduction in the risk of probable dementia. Because of early study termination and fewer than expected cases of dementia, the study may have been underpowered for this end point.”
High Blood Pressure and Dementia:
There is evidence that hypertension in middle age is associated with a greater risk of dementia. How much greater? 60% greater! That was conclusion of a review published in The Lancet (Aug. 8, 2020).
But the authors of an analysis published in JAMA Internal Medicine (Dec. 13, 2021) point out that in late life:
“…this association disappears, with few studies finding associations with increased risk and most studies reporting neutral or even decreased risks associated with hypertension.”
The researchers analyzed seven cohort studies involving 17,286 participants. Their findings will challenge conventional wisdom that less is best. They found that elderly people may actually do better when their systolic blood pressure is higher than the guidelines usually recommend. That’s because the lowest risk point for dementia and mortality combined was 163 mm of mercury for systolic pressure. That is substantially higher than most doctors like to see.
People between 60 and 70 years of age had the lowest risk when their systolic blood pressure was around 135. After age 70, however, the optimal range was 160 to 165. Most cardiologists would cringe at such data.
The Controversy Continues:
What are we to make of this controversial association? The authors acknowledge that a randomized controlled trial found lower mortality and dementia risk among certain people whose systolic blood pressure was reduced below 120. How do we reconcile this contradiction?
To do this, the authors say, we need future studies to:
“…test BP management that is tailored to one’s age, life expectancy, and health context.”
In the meantime, people with hypertension should absolutely consult their health care providers to determine the most appropriate treatment approach to control high blood pressure.
Not the First Rodeo:
This is not the first time data have challenged the 120/80 goal for everyone, regardless of age. In 2017 we posed a question in this article:
Will Low Blood Pressure Increase the Danger of Dementia in Older People?
Is lower blood pressure always better? Many people think that 120/80 is ideal but older people may be at risk for dementia if diastolic BP goes too low.
We cited an Italian study published in JAMA Internal Medicine, April, 2015.
The authors concluded:
“Low daytime SBP [systolic blood pressure] was independently associated with a greater progression of cognitive decline in older patients with dementia and MCI [mild cognitive impairment] among those treated with AHDs [antihypertensive drugs]. Excessive SBP lowering may be harmful for older patients with cognitive impairment. Ambulatory blood pressure monitoring can be useful to help avoid high blood pressure overtreatment in this population.”
You can read about the 90+ Study at this link. It too is a man bites dog story. By now you are probably shaking your head in disgust. Some doctors insist that getting blood pressure below 120/80 should be the goal regardless of age. Others point out that such an aggressive strategy can lead to adverse drug effects such as dizziness and falls. That is especially problematic for older people. A fall can lead to a broken hip, which in turn can lead to disability and early death. A head injury can be devastating at any age. And let’s not forget the controversy about low blood pressure and dementia in older people.
The SONIC Study in Japan:
Japanese researchers began collecting data on older people in their 70s, 80s and 90s starting in 2010. It was called SONIC because it stood for Septuagenarians, Octogenarians, Nonagenarians, Investigation with Centenarians. The volunteers were from eastern and western areas of Japan. Blood pressure and lipid levels were measured. The subjects were also tested for cognitive function by using the Montreal Cognitive Assessment-Japanese version (MoCA-J). The higher the score on the MoCA-J test, the better the brain function.
Data were collected from 2010 till 2012 with a follow-up survey after 3 years. The results were published in the journal Hypertension Research, April 24, 2023. To understand the data you should note that the Japanese researchers defined patients with “dyslipidemia” as those with triglyceride levels greater than 150 and “bad” LDL cholesterol levels over 140. Dyslipidemia basically means “bad” lipid levels.
The authors define hypertension in Japan and the criteria for this study:
“According to the criteria of the Japanese Society of Hypertension guidelines for the management of hypertension (JSH 2014), the diagnosis of hypertension was based on BP values over 140/90 mm Hg and the use of antihypertensive treatment at the time of the first contact.”
We apologize for such detail, but to understand the results of this intriguing study you have to appreciate that the Japanese researchers were defining “dyslipedemia” (bad lipid levels) and hypertension substantially higher than most American cardiologists. One final point. American cardiologists are starting to sour on so-called good HDL cholesterol. Many no longer think raising HDL-C is beneficial.
The SONIC Results Defy American Guidelines.
Here is the bottom line in the authors own words:
“High high-density lipoprotein cholesterol (HDL-C) and diastolic blood pressure (DBP) levels of individuals with hypertension & dyslipidemia and high systolic blood pressure (SBP) levels of individuals with hypertension were associated with maintaining cognitive function.”
What the heck does that mean?
People with high levels of “good” HDL cholesterol, elevated “bad” LDL cholesterol and high diastolic blood pressure readings had “higher MoCA-J scores.” Remember that the higher the Montreal Cognitive Assessment-Japanese score, the better the cognitive function. People with higher systolic blood pressure also scored higher on the MoCA-J assessment tool.
The authors go on to state that:
“According to the lipid level, several previous studies suggested that low HDL-C, low LDL-C, and low T-CHO [total cholesterol] were associated with Alzheimer’s disease around the age of 70 years old.”
“Several studies have investigated the relationship between BP in later life and cognitive function. One of the previous longitudinal studies on the relationship between BP and cognitive function suggested that lower SBP [systolic blood pressure] and DBP [diastolic blood pressure] were associated with a higher risk of Alzheimer’s disease or cognitive impairment. Our study supported these findings of the protective effects of high HDL-C, SBP, and DBP on cognitive function.”
“In older adults, especially at age 90, adequate cerebral perfusion may help to maintain normal cognition.”
We recognize that the Japanese researchers are offering a perspective that would be considered heretical by most cardiologists and neurologists in the United States. We will not add any commentary.
Our recommendation: each person must be treated individually. Following a one-size-fits-all-guideline is not good medicine.
What Causes Hypertension?
At the danger of oversimplification, it may be helpful to think about blood pressure in terms of plumbing. Think of the heart as a pump with hoses connected to it. In actuality, there is one main outflow hose (the aorta) that connects to lots of smaller branching hoses (arteries) throughout the body. Each time the heart contracts to push blood through the system, pressure in the outflow hoses reaches a peak, called the systolic pressure. As the heart relaxes, the pressure lets up. That’s called diastolic pressure. Because early pressure-measuring devices used a column of mercury, blood pressure is expressed in units of milimeters of mercury (mm Hg). The systolic is first and the diastolic second: 120/80, etc.
Now, think about a garden hose and imagine that the water is just pouring out without much pressure. If you held the hose in your hand the water might only reach a few feet. To get a strong flow, you need a nozzle to narrow the opening. The smaller the nozzle, the farther and harder the water will shoot.
Blood vessels operate in a somewhat similar manner. Healthy blood vessels are flexible and can change their diameter by contracting or relaxing. When the diameter narrows, as it does under stress or excitement or as a consequence of atherosclerosis, the pressure inside the vessel increases. Atherosclerosis (aka hardening of the arteries) makes the vessels stiff so they cannot dilate and lower blood pressure.
If pressure inside the circulatory system gets too high, organs such as the brain, the heart, or the kidneys may suffer. Equally, if blood pressure drops too low, not enough blood carrying oxygen or nutrients can get to vital organs. When people go into septic shock because of a serious blood infection, their blood pressure drops dramatically. Without adequate blood flow, kidneys and other organs can fail.
Blood pressure can vary significantly throughout a normal day or week—by as much as 50 points over the course of 24 hours. Exercise or agitation makes it rise; meditation, deep breathing or sleeping usually makes it drop. The levels at which a doctor decides that blood pressure requires treatment are somewhat arbitrary, and may be different from one doctor to the next.
White Coat Hypertension
White coat hypertension is the medical term for a reaction some people have to the approach of a doctor or nurse with a blood pressure cuff. The pulse may quicken and blood pressure soar 20 or more points right in the doctor’s office.
The best study of this was done some years ago in Italy with equipment that took extremely accurate, continuous blood pressure measurements on 48 hospitalized people (Lancet, Sept. 24, 1983). The researchers actually placed a catheter in the radial artery of the arm to directly measure blood pressure. When a physician entered the room, 47 out of 48 patients experienced a dramatic increase in BP within one to four minutes. The average systolic rise was 27 points, but one reading spiked 75 mm. Even people with normal blood pressure had substantial elevations when a doctor entered the room.
Many physicians find the phenomenon of white coat hypertension hard to handle. They think of themselves as healers. How could a doctor’s presence provoke such a dramatic alarm reaction in a patient? It’s challenging for health professionals to contemplate that they are scaring their patients.
White coat hypertension is controversial. Some physicians believe that it should be treated aggressively, on the grounds that any stress may make blood pressure rise excessively in someone who experiences it. They reason that if a person has hypertension in the doctor’s office, he or she may respond in a similar way to a disagreement with the boss, an argument with a spouse, or a close call in traffic.
Other doctors fear that white coat hypertension may lead to false diagnoses of disease, as our blood pressure is constantly changing throughout the day and week. Being labeled “hypertensive” is enough to affect self-image, work productivity, and general well being. It may also result in unnecessary medication.
A systematic review of studies of white coat hypertension in the Annals of Internal Medicine (June 18, 2019) concluded that untreated white coat hypertension was associated with increased risk of cardiovascular events. Another review reported that blood sugar may be a confounding factor (Clinical and Experimental Pharmacology & Physiology, Jan. 2014): “In conclusion, management of a patient with WCHT [white-coat hypertension] should focus on cardiovascular risk factors, particularly glucose intolerance, not blood pressure alone.”
How many people are affected by white coat hypertension? We have been disappointed to discover that this important question has not been studied as rigorously as you might imagine. Some experts estimate that 15 to 30 percent of patients diagnosed with high blood pressure may have a problem only in the doctor’s office. One study titled “How Common Is White Coat Hypertension?” was published in JAMA (Jan. 8, 1988). It concluded that 21% of clinic patients with white coat hypertension had normal blood pressure outside the clinic.
We encourage people to acquire an easy-to-use home blood pressure monitor and to keep a diary of readings that can be shared with a health care provider. This way, people can measure their blood pressure under a variety of conditions (work, stress, relaxation, etc.), which can help determine the most appropriate treatment strategy. There are also accurate home devices that can send blood pressure readings to a home computer or a smart phone or directly to a doctor’s office.
Home Monitors
We remember when physicians believed measuring blood pressure was way too complicated for most patients to master. That was a time when doctors monitored blood pressure with an arm cuff they pumped up and then watched a column of mercury descend in a glass tube. They had to listen attentively with a stethoscope for “Korotkoff sounds” as the pressure in the arm cuff was gradually lowered. The mercury tube was eventually replaced with a round guage.
Listening for subtle sound changes through a stethoscope applied to the brachial artery in the crook of the elbow requires good hearing. Older male physicians often have hearing loss, but they rarely admit it to themselves or others. Researchers actually studied hearing capability in over 100 physicians and med students (American Journal of Otolaryngology, Jan.-Feb. 2006). The authors reported that “46% of physicians with hearing loss described their hearing as good.” The conclusion: “Physicians lose hearing with age but may not notice or report the loss.”
It has been established that hearing loss leads to inaccurate blood pressure measurements (Blood Pressure Monitoring, Feb. 2014): “When measuring blood pressure with hearing loss, the SBP [systolic blood pressure] tended to be underestimated and the DBP [diastolic blood pressure] was overestimated.”
Nowadays, most clinics rely on automated devices that self inflate and produce a digital readout. It seems rare for a physician or even a nurse to take a patient’s blood pressure. More likely a technician who knows little about proper technique will slap a blood pressure cuff on your arm and hit a button. It should now be obvious to everyone that patients are quite capable of taking their own blood pressure. In fact, there is a good chance that their measurements will be more reliable than those taken in a doctor’s office or a hospital.
There are so many home blood pressure monitoring devices on the market that it is hard to keep up. Most devices are self-inflating, making it possible for anyone to take his or her own blood pressure without assistance.
We have been especially impressed with the Omron products. They are easy to use, accurate and reliable. Consumer Reports has been rating Omron devices favorably for decades. At the time of this writing the model that is most highly rated by CR is the Omron 10 Series BP786N. It costs somewhere between $55 and $95 depending upon where you shop. The molded flexible arm cuff fits arms with a circumference of 9 to 17 inches. That covers most people. Two individuals can store their data on the device, send the results to a smart phone and share them with a doctor’s office via email.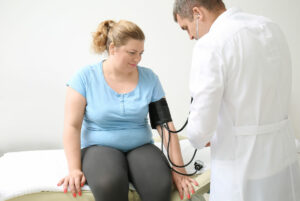
To Get An Accurate Reading
You might be amazed how frequently mistakes are made when blood pressure is measured in a doctor’s office, clinic or hospital setting. For example, the picture of the woman having her blood pressure taken has examples of serious errors. How many can you count?
Take Time to Relax
Going to the doctor’s office, a medical clinic or a hospital can be stressful. Fighting traffic, finding a parking place, checking in and then waiting for a very long time can take a toll. When a nurse or technician finally calls your name, whisks you back for weight, blood pressure and temperature recording, you can feel pretty tense. Whether you take your BP at home or have it measured in a clinic setting, you should always take 5 to 10 minutes to sit and relax prior to any reading.
Take a Bathroom Break Before BP Measurements
Are you encouraged to go to the bathroom before someone measures your blood pressure? A full bladder can increase both systolic and diastolic blood pressure readings (Korean Journal of Family Medicine, July, 2011).
Get in the Proper Position
Does the person who measures your blood pressure always provide you with a comfortable chair? Does it have a back rest? Are your feet flat on the floor? Is your arm always supported at heart height either by an arm support or by the person who takes your blood pressure reading? These are the guidelines set up by the American Heart Association. As you can see by the photograph above, all of these rules have been broken. Error # 1: this woman is sitting on an exam table with no backrest. Error # 2: her feet are dangling. Error # 3: her arm is at her side. If your arm is in your lap, both your systolic and diastolic numbers will be higher. All these errors could contribute to inaccurate BP readings.
Use the Proper Cuff Size
Error # 4: the woman above has large arms. It is entirely possible that the cuff is too small. Have you ever had a doctor, nurse or clinician measure your arm circumference? We didn’t think so. A cuff that’s too small could falsely elevate your readings. Request the right cuff size at the doctor’s office. And if you need a larger cuff at home, Omron makes them in a variety of sizes.
Avoid Talking
Doctors and nurses often like to chat with patients during readings because they think it will help calm us down. Research suggests, however, that they may elicit the opposite reaction (Angiology, July, 1982). A measurement taken during conversation could be artificially high (more than 20 points!). Try to sit quietly for 5 minutes before your blood pressure is taken. Never respond to questions or idle chit chat while your blood pressure is being taken!
Make Sure There Are Multiple Measurements
Did the nurse, technician or physician measure your blood pressure at least twice during your visit? One solitary reading is not adequate. It is recommended that a minimum of two measurements be made with some time between readings. The data can be averaged to better represent your blood pressure at that particular moment.
Keep a Diary
There is enormous variability in blood pressure throughout the month, the week and even the day. The numbers that get recorded in your chart are only one tiny sliver of your blood pressure story. Imagine if your life were a big book containing 1000 pages. A blood pressure measurement in a doctor’s office is like one sentence out of that entire big book of life. Trying to interpret even a few readings is risky.
For that reason, it’s important to take blood pressure readings at various times of day and under as many different conditions as possible. Keep a careful record of your readings and of what you were doing before and during each measurement. That will help you note trends that you can then share with your physician.
If you really want the most accurate blood pressure assessment you will need to ask your doctor to prescribe a portable (ambulatory) monitoring device. It takes your blood pressure every 20 minutes during the daytime and every 30 minutes during the night. A Spanish study involving nearly 64,000 patients for a decade revealed that ambulatory blood-pressure measurements were a better predictor of cardiovascular mortality than clinic measurements (New England Journal of Medicine, April 19, 2018).
Non-Drug Options
There are literally dozens of medications for high blood pressure on the market, and while pharmaceuticals may indeed be the only option for some people, all of these pills can cause side effects, sometimes very serious ones like potassium depletion.
We think it can’t hurt to try some non-drug options first. Remember, though, that it’s extremely important to communicate with your physician at every stage about blood pressurelowering strategies. Managing hypertension requires careful medical supervision.
Are You Angry?
Drs. Redford and Virginia Williams wrote a fabulous book several years ago called Anger Kills. Their work reveals that hostility is bad for the heart.
There’s also confirming evidence from Canadian researcher J. David Spence, MD, that people who react to stress and frustration with elevated blood pressure may be more likely to develop atherosclerosis than people who take life’s curveballs in stride. These “hot reactors” may be at least as vulnerable to hardening of the arteries as people who smoke or have diabetes. Dr. Spence believes that people who overreact to stress may be a lot like hostile and cynical folks who are also at greater risk of heart attacks and strokes.
If you’re someone who tends to feel stressed or angry when you’re cut off in traffic, your spouse is late for dinner, or a person in the express lane at the supermarket has too many items, you might want to think about learning to recognize and monitor your tense reactions, as they could be negatively affecting your health.
Watch your weight
Losing as little as 10 or 15 pounds can make a big difference in your blood pressure. Overweight people who shed about 18 pounds can expect their systolic blood pressure to drop by 8.5 mmHg and their diastolic pressure to come down by 6.5 mmHg. That’s about what you could hope for if you were to go on medication. Of course, losing weight may be difficult, but it is well worthwhile in terms of self esteem and general health.
The experts tell us that many people munch when they are bored, anxious or upset, and that this contributes to unconscious calories that can really add up. A food diary is a good way to review when you are eating and why. The very act of writing down every bite can make you more aware of your mental state and encourage alternative activities for relaxation or relief of boredom.
Sensible eating usually means less fat and more fresh fruits, vegetables and whole grains. We especially recommend the DASH (Dietary Approaches to Stop Hypertension) diet (see right), but keep in mind that different programs work for different people. And of course, portion control is important, too. One trick we like when we eat out is sharing the entree. If your dining partner is willing, this can halve your restaurant calories.
The other component of a weight loss program is to increase the energy you use. Engaging in regular, moderate exercise can help bring down blood pressure by at least 2 or 3 mmHg. For starters, try parking a little farther away at work or the shopping mall.
Measuring Stress
We started this blood pressure guide with the statement that hypertension is a silent killer. That’s because we 1) cannot determine our blood pressure without a device and 2) we cannot sense gradual organ damage.
Stress can affect our blood pressure but not everyone is good at assessing their internal stress level. Would you like an easy strategy for doing just that?
If you lived through the 1970s, you probably remember the mood ring craze. Silly as it may sound, mood rings (or their newer, higher-tech cousins) might provide a good visual cue for rising stress levels that could signal elevated blood pressure. By the way, mood rings are still readily available online.
There’s a Bio-Q Thermal Biofeedback and Stress Monitoring Ring. If you don’t like rings, there are liquid crystal “chips” smaller than stamps. Look for Stress Squares or Biodots that you can stick to your skin. Like the rings, they change colors as your body temperature (and mood) changes. Some smart watches can also monitor your stress level.
If you find your biofeedback device is telling you that you are under stress, try to exit the situation. It’s not good for your health.
Exercise sensibly
If you are out of shape, never start exercising without first checking with your health care provider. Overdoing it, especially in the beginning, is the path to disaster. One study revealed that people who were out of shape and unprepared were 100 times more vulnerable to a heart attack if they suddenly started to exercise vigorously. Shoveling snow or running to catch an airplane can trigger serious heart problems.
Pick an activity that you enjoy. That way you are more likely to stick with it. Walking is excellent, especially if you can do it for 30 to 60 minutes at least four days a week. Whatever exercise you select, keep it up. The buddy system can be a great motivator if your friend encourages you. Make sure to put your exercise times on the calendar as if they were important appointments. Fitness will improve and weight loss will follow.
Eat Drink and Be Merry
The DASH Diet
Designed specifically to help control hypertension, the DASH diet has been studied extensively and demonstrated to be effective. It brings systolic pressure down by an average of 11.4 mmHg and diastolic by 5.5 mmHg. The basics are daily intake of:
- 4 servings of fruit
- 4 servings of vegetables
- 7 to 11 servings of grains
- 2 to 3 servings of low-fat dairy foods
- Nuts, fish, and poultry
- Little red meat, sweets, and sugary drinks
For $8, you can get more specifics from the book The Dash Diet for Hypertension, or for free, you can get an overview at this link.
Remember, though, that other diets may work just as well. In fact, research from Johns Hopkins suggests that replacing some of the carbohydrate calories in the DASH diet with protein or monounsaturated fats may be even more effective for lowering blood pressure and cholesterol. Choose the diet that’s right for you—South Beach, the Zone, or something else that better fits with your lifestyle.
Maximize Your Minerals
Minerals can make a difference for blood pressure and heart health. Calcium, magnesium and potassium are especially important. While the individual effects of each of these electrolytes on blood pressure is relatively small, studies have shown that together they can have a significant impact. Of these three, magnesium may be the most essential, in part because it’s often lacking in our diets. This is often especially true for those on diuretics, as these drugs can deplete people’s systems of magnesium (and potassium).
Get your minerals from food if possible. Taking supplements could result in an overdose, but that is difficult when eating fruits and veggies. As an extra benefit, you are more likely to get adequate amounts of folic acid, which is helpful for the heart.
For a list of magnesium-rich foods, see the sidebar to the left. Foods high in potassium include: apricots, artichokes, asparagus, bananas, beets, bell peppers, blackstrap molasses, broccoli, brussels sprouts, buttermilk, cabbage, cantaloupe, carrots, cauliflower, chicken, fish, kidney beans, lentils, lima beans, nectarines, oatmeal, onions, oranges, peaches, plums, pomegranates, potatoes, prunes, raisins, raspberries, wheat germ, and yogurt.
Special Foods
Although the jury’s still out on whether or not garlic and onions really lower blood pressure as many people claim, it certainly can’t hurt to try adding them fresh to your diet. Be careful about garlic supplements, though: they may interact with some medications to increase the risk of bleeding.
Another food some folks swear by is celery. Again, there’s no scientific evidence to prove it can fight hypertension, but it’s worth a try. The “dose” is eight ribs a day; do an experiment and record your blood pressure readings to see if you notice a change.
Some other foods may block angiotensin-converting enzyme just like the ACE-inhibitor class of drugs: compounds in aged gouda and fermented milk products like kefir, which you can get in health-food stores.
High Magnesium Foods
Halibut, 3 oz (90 mg)
Almonds, 1 oz (80 mg)
Cashews, 1 oz (75 mg)
Soybeans, ½ cup (75 mg)
Spinach, ½ cup (75 mg)
Mixed nuts, 1 oz (65 mg)
Shredded wheat, 2 (55 mg) Oatmeal, 1 cup (55 mg)
Baked potato (50 mg)
Peanuts, 1 oz (50 mg)
Black-eyed peas, ½ cup (45 mg)
Yogurt, plain skim, 8 oz (45 mg)
Brown rice, ½ cup (40 mg)
Lentils, ½ cup (35 mg)
Avocado, ½ cup (35 mg)
Banana, (30 mg)
recommended: 250-500 mg
Chocolate
Hard as it may be to believe, chocolate can actually be good for your health (Frontiers in Nutrition, Aug. 2, 2017). It’s full of the same antioxidant flavonoids found in red wine and green tea—in fact, cocoa and chocolate have even more of the good stuff, as well as other compounds that help the heart and cardiovascular system. One long-term study showed that Dutch men who ate about 10 grams of chocolate a day (the size of a Ghiradelli square) had lower systolic pressure by 3.7 mmHg. Their chances of dying of heart disease during the study were also decreased by 50%.
Go ahead and try a little chocolate—the taste (and rewards) are sweet! Remember that for maximum benefit you want minimum sugar; probably chocolate with at least 70% cocoa content will work best. If you’re watching your blood sugar or calories, you could go for cocoa without sugar, like Scharffen Berger or Valrhona (not alkali or Dutch-processed).
Don’t count on chocolate alone to lower your blood pressure. Although researchers have found that people who eat more chocolate seem to have a slightly lower risk of coronary heart disease or stroke (complications of high blood pressure), they warn that the evidence is not of high quality (European Journal of Nutrition, Feb. 25, 2019).
The Dirt on Salt
If you have high blood pressure, you’ve probably been told for years to avoid salt. But despite the ubiquity of this advice, the story on salt and hypertension is confusing at best and contradictory at worst.
A comprehensive review in the New England Journal of Medicine (Nov. 18, 2021) reveals how challenging the salt-blood pressure connection really is. For one thing, your body is exquisitely capable of regulating sodium balance. In other words, under normal conditions your body controls sodium by excreting (peeing) the excess.
The authors of the article titled Insights into “Salt Handling and Blood Pressure” point out that:
“…high salt intake raises blood pressure. Yet many persons are able to consume large amounts of salt without substantial rises in arterial pressure. A recent Cochrane review showed that dietary salt restriction, as compared with high salt intake, reduces mean arterial pressure by 0.4 mm Hg in normotensive persons and by 4 mm Hg in those with diagnosed hypertension.”
Lowering BP 4 points is not nothing. But it’s also not a dramatic improvement. And it turns out that there is substantial person-to-person variability. Some people are quite salt sensitive, whereas others can eat a fair amount of salt and not suffer an increase in blood pressure.
Potassium to the Rescue:
It turns out that potassium is a key player in the salt wars. Another article in the New England Journal of Medicine (Sept. 16, 2021) reveals the crucial role potassium plays in helping regulate blood pressure. A large randomized controlled trial tested a salt substitue containing 75% sodium chloride and 25% potassium chloride against 100% sodium chloride (table salt). The volunteers who used the salt substitue had lower blood pressure and fewer strokes or major cardiovascular complications.
People should not go wild with salt. But new research suggests that avoiding salt as much as possible may not benefit longevity as much we’ve all been told. We encourage you to eat salt with moderation, especially if you’re salt-sensitive. But your quality of life doesn’t have to suffer entirely, either.
Dietary Supplements
There isn’t a lot of hard evidence to suggest that supplements can dramatically reduce blood pressure, but there’s some data that seem to indicate coenzyme Q10 might be somewhat effective. Another supplement that may prove beneficial, especially for those who are prehypertensive, is grape seed extract. In one study, subjects taking it saw a 12-point drop in systolic BP and an 8-point decrease in diastolic.
Beet Juice
Research out of England suggests that beet juice may be at the vanguard of the blood pressure battle (Hypertension, March 2008). Volunteers in a study were given either two cups of beet juice to drink or two cups of water. Those who drank the beet juice experienced about a 10-point drop in blood pressure readings, and the effects lasted for a whole day. These results are as good as those you could expect from many drugs.
This research has been cited by more than 100 other medical publications. Scientists have found that even healthy people have lower blood pressure a few hours after drinking beet, spinach or arugula juice (Journal of Nutrition, May 2016). Beets are not the only vegetables that can increase nitrate levels in the blood vessels, relaxing the lining and lowering blood pressure. High-nitrate vegetables include arugula (rocket), chervil, celery, spinach, collard greens, red beets (and their greens), lettuce, leeks and watercress (Methodist DeBakey Cardiovascular Journal, Jul-Sep. 2019). All of these can help reduce stress on the heart and blood vessels.
If you don’t have a juicer and you’re having trouble finding beet juice in your local health-food stores, you can always order it online. Retailers like www.truefoodsmarket.com carry beet juice, but there are many others.
Beet Juice Lemonade:
For people who are not fond of plain beet juice, we have a recipe for beet juice lemonade. It looks beautiful and tastes terrific:
- Put 1 small to medium-sized peeled chopped beet in a blender with 3 T water.
- Dissolve 1/2 cup sugar in 6 cups of water. Do this in a pan on a stove over medium heat. Let the sugar solution cool completely.
- Squeeze the juice from 3 lemons. Add it to the sugar solution.
- Strain the blended beet juice into the lemonade solution. Chill before serving.
Pomegranate Juice
If you like sipping juice but hate beets, there are some other liquid alternatives for fighting hypertension. Pomegranate juice has a consistent blood pressure lowering effect (Pharmacological Research, Jan. 2017). Apparently, pomegranate compounds act sort of like an ACE inhibitor to block the angiotensin-converting enzyme, thus lowering blood pressure (Atherosclerosis, Sep. 2001). It can reduce ACE activity by roughly 36% percent, and one study found that subjects who drank 2 ounces of it daily brought their systolic pressure down by about 8 points.
Pomegranate juice also benefits the cardiovascular system in other ways, by reducing the risk of blood clots and improving blood-flow and oxygen delivery to the heart. It also lowers total and bad LDL cholesterol. In general, the juice from these tiny seeds seems to create big results.
Concord Grape Juice
And finally, purple grape juice may be another blood pressure-lowering beverage. In one study, it brought systolic BP down by about 7.2 points and diastolic by 6.2. Grape juice can also lower cholesterol, improve blood vessel flexibility, and decrease the risk of blood clots. The suggested amount is about two glasses per day. Grape juice has a lot of sugar and calories, though, so we don’t recommend it to those watching their weight or sugar intake.
Socialize and Be Merry
One very pleasant solution to the problem of hypertension is to maintain close ties to family and friends. Loneliness is a risk factor for high blood pressure: it can raise readings by up to 30 points. It may also contribute more to cardiovascular disease than even obesity or lack of exercise. Isolation can strike those of retirement age especially hard; at least 9 million Americans over the age of 50 are believed to frequently feel lonely. Nurture your social networks, and try creating new ones: volunteer work, art or dance classes and bringing home a new pet are ways to maintain a sense of connection.
Learn to Relax
Relaxation, whether you get it from listening to soothing music or petting the family cat or dog, is one of the most delightful and effective ways of lowering blood pressure. So many Americans are living in the fast lane that lots of people have forgotten how to relax. Biofeedback can be helpful for folks with high blood pressure. Another approach is listening to relaxation tapes, such as those from Emmett Miller, M.D. Try “Down with High Blood Pressure.”
Emmett Miller’s Tapes available from: www.drmiller.com Or by calling: 800 528-2737
Enjoy a Good Soak
One popular way to unwind is with a nice long soak in a hot mineral spring. It turns out that regular use of a hot spring or sauna can be a good way to help keep your blood pressure under control. A recent meta-analysis of 12 studies, including a total of 1122 participants, found that those who immersed themselves in thermal springs had positive effects (International Journal of Biometeorology, Dec. 2019).
Sauna Bathing
Finnish researchers have been studying the health benefits of sauna bathing for years. Sitting in a hot wooden room has been a tradition in Finland for thousands of years. A study published in the Mayo Clinic Proceedings (Aug. 2018) reviews the evidence for cardiovascular and other health benefits. These include improvements in circulation and a reduction in cardiovascular risk factors.
People with high blood pressure see a reduction in both systolic and diastolic blood pressure after sauna bathing. Studies also indicate that this practice may reduce the risk of dementia, lung disease, mental disorders and pain. Perhaps the rest of the world should pay attention to this ancient Finnish tradition. Some Americans who have tried it are enthusiastic.
A twenty-year study of more than 2,000 men in Finland found that frequent sauna bathing was associated with a lower risk of sudden cardiac death (JAMA Internal Medicine, April 2015). When the men volunteered for the study in the 1980s, they filled out questionnaires about whether they visited the sauna two or three times a week, every day, or only once a week. Only 12 men in this study never went to the sauna.
Follow-up showed that 10 percent of those using the sauna weekly died of sudden cardiac death during the study, compared to only 5 percent of those who went every day. The pattern held up for death from other cardiovascular causes, and daily sauna bathers were also less likely to die from any cause during the study time frame. Finnish saunas use dry heat, so the results might not hold for steam baths.
Breathe Easy
This may sound obvious, but learning to breathe deeply and well can really reduce blood pressure. It’s harder for some people to do than you might think. One way to bone up on your breathing technique is to try meditation or yoga.
If yoga’s not for you, though, another amazing method is to practice slow breathing. A review of 17 studies found that if people practice taking 10 or fewer breaths per minute for at least five minutes three times a week or more, they can lower their blood pressure by around 6 mm Hg over 3 mm Hg (Complementary Therapies in Medicine, Aug. 2019). You can’t just do this once, though. It needs to be continued over weeks and months.
If this is more discipline than you can muster, you might find it easier with a device. Apple watch and doubtless some other watches have a slow breathing app built in. Or you could try a machine called RESPeRATE. It consists of a chest strap, a set of earphones, and a computerized device about the size of a thick paperback. Initially, you breathe into it normally so that its sensors can learn your breathing pattern. But eventually this breathing “coach” uses melodious tones to prolong your exhalations. Ideally, you want to get down to 10 breaths per minute. Studies have shown that RESPeRATE can decrease blood pressure by at least 5 points, and perhaps by as much as 10 or 15.
But one downside is that RESPeRATE requires a significant time commitment— about 15 minutes per day at least four or five times a week. It’s also quite pricey (around $300), so you shouldn’t invest in it unless you’re ready to use it regularly. And exercise will likely work at least as well.
RESPeRATE Available at: www.resperate.com or 877-988-9388
Quit Smoking
Too obvious to belabor. And of course, this will make breathing deeply much easier. One caution, however: we are a bit leery of stop-smoking drugs like Chantix, as they seem to produce a host of negative side effects that worry us, including depression and suicidal ideation. When you do make the decision to quit, work with your doctor and loved ones to come up with a plan that you can stick to.
Other Things to Avoid
Coffee and Soda
The relationship between caffeine and hypertension isn’t necessarily straightforward. While some research suggests that as little as a cup of coffee can modestly increase blood pressure, it may not be a problem for all people. Those who should watch out, however, are folks who metabolize caffeine slowly. If you find that the cup of coffee or can of soda you drank in the afternoon can keep you tossing and turning at night, you’re probably a slow caffeine metabolizer. Slow metabolizers seem to be at considerably higher risk of heart attack—the more caffeine they consume, the higher the risk. It’s hard to be certain what kind of metabolizer you are, so we advice cautious consumption of caffeine for all those with blood pressure concerns.
And it may not only be caffeine that’s a problem. A large study of nurses showed that those who drank soda (diet or regular) had a higher rate of hypertension. The researchers didn’t think caffeine in the sodas was responsible, but most likely something else (as yet unidentified). It’s probably also wise, then, to go light on the cola.
Green or oolong tea might make a very good substitute for coffee and soda: they appear actually to lower blood pressure.
Licorice
Black licorice may sound like a surprising culprit for hypertension, but this tasty treat can really throw your metabolism out of whack, imbalance hormones, deplete potassium—and elevate blood pressure significantly. So if you’ve been heavyhanded with the Good & Plentys, it might be time to lay off a bit.
Pain Relievers and NSAIDs
Have you ever felt as if you were driving with your foot on the brake and the gas at the same time? If you are caught in stop and go traffic, you know how frustrating it can be. It’s hard to get very far in such a situation. That’s what happens when you are prescribed a drug to help control hypertension while you are simultaneously taking medications that raise blood pressure. You might be surprised to learn how many prescription and OTC meds can contribute to hypertension.
People in pain frequently turn to NSAIDs for relief. That is especially true ever since physicians and pharmacists became worried about prescribing or dispensing opioids.
According to the publication U.S. Pharmacist (March 17, 2016):
“It is estimated that more than 30 million people use these drugs on a daily basis, and they account for 60% of the analgesic market in the United States.”
We’re talking about over-the-counter ibuprofen (Advil, Motrin IB, etc) and naproxen (Aleve).
Doctors prescribe drugs such as ibuprofen, meloxicam (Mobic), naproxen (Naprosyn), celecoxib (Celebrex), diclofenac (Voltaren) and indomethacin (Indocin). At last count, over 70 million prescriptions for such NSAIDs are filled annually in the United States.
A study published in Pharmacoepidemiology & Drug Safety (Jan. 26, 2018) reports that:
“• 15% of adult ibuprofen users in the US exceed the maximum recommended daily dose of 1 or more over-the-counter or prescription NSAIDs during a week in which they use ibuprofen. The maximum was exceeded on 9.1% of usage days, and on 20% of days with more than 1 usage occasion.”
It was not unusual for people taking ibuprofen to also take naproxen.
Perhaps more alarming, the study found that:
“The daily limit for naproxen was exceeded by 23% of users of that drug, a significantly higher prevalence than for ibuprofen, and almost all with OTC products.”
NSAIDs Are Medications That Raise Blood Pressure:
People often assume incorrectly that most over-the-counter drugs are quite safe. Why would the FDA approve them for such use if they weren’t relatively harmless?
Some Popular NSAIDS:
- naproxen (Aleve, Anaprox, Naprosyn)
- diclofenac (Voltaren, Cataflam)
- celecoxib (Celebrex)
- meloxicam (Mobic)
- indomethacin (Indocin)
- piroxicam (Feldene)
- Sulindac (Clinoril)
We have heard from many readers that NSAIDs contribute to higher blood pressure. They are not always warned:
“After diagnosing my arthritis, my doctor prescribed meloxicam. During the three years I took it, my blood pressure went from 120/80 to 190/144. Unfortunately, he wasn’t monitoring it.
“When I found I had such high blood pressure, I got off the meloxicam and was put on lisinopril. Six months later, my BP is stable at 130/86. I do want it lower, so the fight is still on. Please monitor your blood pressure while you are on meloxicam.”
The FDA mandates the following warning with meloxicam and other NSAIDs.
“NSAIDs, including meloxicam, can lead to onset of new hypertension or worsening of pre-existing hypertension, either of which may contribute to the increased incidence of CV [cardiovascular] events. Patients taking thiazides or loop diuretics may have impaired response to these therapies when taking NSAIDs. NSAIDs, including meloxicam, should be used with caution in patients with hypertension. Blood pressure (BP) should be monitored closely during the initiation of NSAID treatment and throughout the course of therapy.”
Preparation H
You may also be surprised to learn that this popular hemorrhoid medication can lead to elevated blood pressure. It contains the decongestant phenylephrine, which constricts swollen blood vessels. There are warnings on the packaging not to use Preparation H if you’re taking blood pressure medication, but one of our readers had some very unpleasant episodes before he discovered the fine print.
Preparation H and High Blood Pressure
“After using Preparation H for several days, my blood pressure went to 206 over 98 and I ended up in the emergency department for hours.
“Later that week I read in your column that someone else had experienced the same problem. My doctor was skeptical, to say the least, so I lent him the clipping.
“I never had high blood pressure before in my life. It was always around 130 over 65.”
Other Medications That can Raise Blood Pressure
There are hundreds of other medications that can make it difficult to manage blood pressure. You might think that physicians would be extremely careful not to prescribe such drugs to people with hypertension. You would also hope that pharmacists would warn patients about OTC drugs or drug interactions that could make it harder to control blood pressure. A study published in JAMA Internal Medicine (Nov. 22, 2021) involving 27,599 patients reveals something quite alarming, however:
“In this nationally representative survey study, 18% of US adults with hypertension reported taking medications that may cause elevated BP. The use of these medications was associated with increased odds of uncontrolled hypertension among individuals not taking antihypertensives and greater use of antihypertensives among both patients with controlled and uncontrolled hypertension.”
Put another way, many people with high blood pressure were trying to climb steps with lead overshoes on. They had hypertension but were also taking medicines that could increase their blood pressure. We cannot list all of the medications that can raise blood pressure in this eGuide. Your eyes would glaze over. Here are some categories that pose problems (JAMA Internal Medicine, Nov. 22, 2021).
- Antidepressants
- Corticosteroids
- Estrogens
- Testosterone
- Stimulants
- Decongestants
- Weight loss medications
Always ask your physician and your pharmacist if a new prescription will raise blood pressure! While you are at it, ask them if anything you are currently taking could make it harder to control your BP. We don’t want you climbing steps with lead overshoes on your feet!
Will the Pharmacist Voluntarily Warn About Medications That Raise Blood Pressure?
Corticosteroids Are Medications That Raise Blood Pressure:
Corticosteroids such as methylprednisolone or prednisone can also raise blood pressure. One study found that hypertension was a relatively common complication of long-term use (Current Medical Research and Opinion, Aug. 2018).
How common is “relatively common”? In one study, 40% of the patients treated with prednisolone for three months developed hypertension (Hormozgan Medical Journal, June-July, 2017). None of the patients had high blood pressure at the beginning of the study.
Are Antidepressants Medications That Raise Blood Pressure?
Antidepressants have also been associated with higher blood pressure. French researchers report that drugs such as citalopram, escitalopram, fluoxetine, paroxetine and sertraline may make it harder to control hypertension (Fundamental & Clinical Pharmacology, June, 2019).
The authors conclude:
“This study, performed in real conditions of life, shows a significant pharmacovigilance safety signal between the use of SRIs [serotonin reuptake inhibitors] and the development or worsening of hypertension.”
The FDA seems unaware of this potential complication. It does not list hypertension as a side effect of Prozac (fluoxetine) except in an overdose situation.
Decongestants Are Medications That Raise Blood Pressure:
Over-the-counter decongestants can also raise blood pressure. Phenylephrine, often abbreviated PE, is found in many popular allergy and cold medicines. It is also found in some nasal sprays and hemorrhoid preparations. The latter may come as a surprise to many readers.
Certain other common products can also raise blood pressure. One surprising item is mouthwash.
Mouthwash May Raise Blood Pressure:
Q. It was fascinating to read in a recent column that mouthwash might raise blood pressure. I found that is true in my own case, though I realize each person is different.
Coffee also elevates my blood pressure. What other common foods or OTC pharmaceuticals might raise blood pressure? I’m trying my best to avoid such things, but it would help to know what they are.
Why Antiseptic Mouthwash Could Cause Trouble:
A. The antiseptic mouthwashes you are referring to kill a variety of oral bacteria. There is growing recognition that the ecology of the mouth is important for good health. Although the benefits and risks of antiseptic mouthwash remain controversial, some experts worry that disrupting the mouth microbiome may increase the risk for cardiovascular complications (Intensive Care Medicine, Jan. 2021).
Bacteria that convert nitrate from foods like spinach or beets into nitric oxide help control the flexibility of blood vessels (International Journal of Molecular Sciences, Oct. 13, 2020). Products that interfere with this conversion appear to raise blood pressure.
Snack Foods Can Raise Blood Pressure:
Processed foods high in salt and sugar are prime suspects. Young people with elevated blood pressure that has not crossed the threshold into hypertension are more likely than their peers to indulge in fast foods, especially salty or sweet ones (Journal of Basic Clinical Physiology and Pharmacology, Dec. 18, 2013). Diets rich in fruit, vegetables, whole grains, legumes and nuts seem to help lower blood pressure (Advances in Nutrition, Jan. 15, 2016).
Be sure to speak with your physician about all of the prescription and OTC pills that you’re taking, and to always read the information provided for each. Otherwise, your efforts to lower your blood pressure might be less effective than they should be.
Diuretics
Potassium Wasting
Diuretics (“water pills”) have long been considered a first step in treating high blood pressure, as they’re extremely safe and effective. When first introduced, they started a revolution in hypertension treatment, and they were once among the most prescribed drugs in the world. But as beta-blockers, calcium channel blockers, ACE inhibitors and angiotensin receptor blockers came on the market, physicians started to overlook diuretics.
Then in 2002, some remarkable results from the government-sponsored study ALLHAT (the Antihypertensive Treatment to Prevent Heart Attack Trial) shook the cardiology world. ALLHAT followed 40,000 patients for several years to test the efficacy of various blood-pressurelowering drugs. Researchers discovered that perhaps the most effective medication for controlling blood pressure was chlorthalidone, an inexpensive diuretic.
Diuretics do have some disadvantages, though. For one thing, they deplete the body of two essential minerals, potassium and magnesium. If these electrolytes drop too low, a person may experience disrupted heartbeat or cardiac arrest. That is why periodic blood tests are crucial. Eating potassium-rich foods (listed on page 4) should help lower this risk. Cholesterol should also be monitored before and during treatment. Some diuretics actually raise cholesterol levels. Indapamide does not have this complication.
Cautions: Anyone allergic to thiazide diuretics, sulfa drugs or oral diabetes drugs should not be taking these medicines. Rash or itching should be reported promptly, as it may be a sign of allergy. If you have kidney or liver disease, lupus or asthma, inform the doctor of your condition, as certain diuretics may make your situation worse. In some cases these drugs may increase blood sugar or aggravate gout.
Side Effects: Adverse events are uncommon. Increased urination is anticipated, so taking such medicine early in the day may reduce the number of times you have to get up at night to go to the bathroom. Muscle cramps, upset stomach, loss of appetite, diarrhea, dizziness, sexual difficulties, increased susceptibility to sunburn, blurred vision and headache have been reported.
Interactions: Please check with a pharmacist and physician if you combine a diuretic with other medicine. NSAIDs such as Advil, Aleve, aspirin, Indocin, Naprosyn, Orudis, Relafen or Voltaren may reduce the effectiveness of diuretics. This could be especially dangerous if someone were taking Lasix or Bumex for heart failure.
Other drugs that may interact with diuretics include colestipol (Colestid), cholestyramine (Questran), lithium (Eskalith, Lithobid, etc.) and oral diabetes medicines (DiaBeta, Diabinese, Glucotrol, Orinase, etc.). Laxatives may deplete the body of potassium, which could be dangerous in combination with potassium-wasting diuretics.
Digoxin (Lanoxin) is commonly prescribed with diuretics like furosemide (Lasix). But if potassium levels drop below normal, this could become a life-threatening situation.
Diuretics (potassium wasting)
| Bumex | bumetanide |
| Diachlor | chlorothiazide |
| Diucardin | hydroflumethiazide |
| Diuril | chlorothiazide |
| Edecrin | ethacrynic acid |
| Enduron | methyclothiazide |
| Esidrix | hydrochlorothiazide |
| Exna | benzthiazide |
| HydroDIURIL | hydrochlorothiazide |
| Hygroton | chlorthalidone |
| Lasix | furosemide |
| Lozol | indapamide |
| Oretic | hydrochlorothiazide |
Symptoms of potassium depletion
(normal potassium range = 3.5 to 5 mEq/L)
- Muscle cramps
- Difficulty breathing
- Confusion
- Mood changes
- Lethargy, fatigue
- Weakness
- Dry mouth, thirst
- Nausea, vomiting
- Irregular heart rhythms
*Symptoms are not a reliable indicator of potassium imbalance. Blood tests are essential.
No one should ever stop or start taking medicines without careful medical supervision. Remember, your pharmacist can provide valuable information about side effects and interactions! Please report any symptoms to your physician promptly.
Potassium Sparing
In order to counteract the potassiumdepleting properties of some thiazides, diuretics were developed that preserve potassium. Amiloride (Midamor), spironolactone (Aldactone) and triamterene (Dyrenium) are prescribed alone or, even more commonly, in combination with hydrochlorothiazide as Aldactazide, Dyazide, Maxzide and Moduretic.
They have many of the same side effects and precautions as the diuretics discussed above. They may still deplete magnesium, and this crucial mineral should be measured periodically.
One of the biggest problems with these potassium-preserving pills is the potential interaction with the ACE inhibitor category of blood pressure medicines (Aceon, Accupril, Altace, Capoten, Lotensin, Mavik, Monopril, Prinivil, Univasc, Vasotec and Zestril). Because the ACE inhibitors also preserve potassium, levels of this electrolyte could rise dangerously. If a physician prescribes a potassium-sparing diuretic and an ACE inhibitor simultaneously, medical supervision must be extremely meticulous with frequent blood tests. Symptoms of too much potassium include breathing difficulty, weakness, confusion, slow heart rate and heart rhythm changes.
ACE Inhibitors
These blood pressure drugs block an enzyme called angiotensin converting enzyme (ACE). Some are also useful in controlling congestive heart failure. Enalapril and captopril may help preserve kidney function in diabetics as well, and ACE inhibitors may be beneficial for secondary stroke prevention when paired with diuretics.
It’s hard to say which ACE inhibitors are the “best” without head-to-head trials. For reasons that are not entirely obvious to us, lisinopril (Prinivil, Zestril) is the most prescribed drug in this class. The latest data that we have suggests that roughly 20 million Americans swallow this medicine daily. It is one of the most prescribed drugs in the US. We have calculated that another 20 million Americans take a medicine containing an ACE inhibitor (ACEi).
Cautions: Because ACE inhibitors are generally well tolerated, they are widely used. But some people may develop lifethreatening allergies to these drugs. Swelling of the face, tongue, lips and airways can make breathing difficult. At the first sign of such a reaction, emergency treatment is essential. Pregnant women must avoid ACE inhibitors; such drugs can be toxic to the fetus during the 2nd or 3rd trimester. Blood disorders and kidney problems are rare but serious complications of ACE inhibitors. People with kidney or liver disease require dose adjustments and monitoring.
ACE inhibitors may occasionally raise potassium to dangerous levels. For this reason it is important to avoid extra potassium, either as a supplement or salt substitute.
Side effects: Most people do well on ACE inhibitors, but if blood pressure drops too low, some individuals may become dizzy or faint. This is more likely after the first few doses, so extra caution is important early in treatment. A dry, hacking cough can be an unpleasant side effect of ACE inhibitors. If such a cough persists, please tell your doctor.
Other possible adverse effects include rash and itching, stomach upset, headache, weakness, irregular heart beats, fluid retention, sexual difficulties, high potassium, elevated enzymes related to kidney function, and sensitivity to sunburn. Some ACE inhibitors may cause loss of taste sensation. They may also raise circulating levels of uric acid, which could trigger gout.
Interactions: No ACE inhibitor should ever be taken in combination with aliskiren (Tekturna, Tekamlo, Tekturna HCT). Diuretics that spare potassium such as Aldactazide, Dyazide, Maxzide and Moduretic may cause dangerous potassium overload in combination with ACE inhibitors. Other drugs that may interact include aspirin and the arthritis medicines Clinoril, Dolobid and Indocin, the gout medicine allopurinol, lithium, cyclosporine, oral diabetes medicines, and rifampin. Check with your pharmacist and physician regarding any other drug in combination with ACE inhibitors.
One interaction that frightens us because it is so rarely acknowledged is an ACE inhibitor with the antibiotic cotrimoxazole (SMZ-TMP, Bactrim, Septra). This common antibiotic can exacerbate the tendency of these blood pressure pills to increase potassium. Excess potassium is just as dangerous as low potassium, and it can happen very suddenly (BMJ, Oct. 30, 2014). High potassium levels can cause irregular heart rhythms or cardiac arrest. When your heart stops beating you need immediate defibrillation or its curtains!
ACE-Aspirin Interactions
Many physicians are unaware that aspirin may reduce the effectiveness of ACE inhibitors. This may occur at aspirin doses of 325 mg or greater, whereas low doses (100 mg) do not seem to be a problem. See:
Guazzi, M. et al. Clin. Pharmacol. Ther. 1998;63:79-83.
Hall, D. et al. J. Am. Coll. Cardiol.1992;20:1549-1555.
Although it is worth noting this concern, more recent research may have laid it to rest. A trial of more than 2,000 people with heart failure found that aspirin was no more likely than warfarin to be associated with heart failure problems (Journal of the American College of Cardiology. Heart Failure, Aug. 2017). Nearly all of the patients in this study were taking an ACE inhibitor or an ARB, and they were randomly assigned to aspirin or warfarin. The follow-up period extended to six years. Consequently, cardiologists are likely to conclude that combining aspirin with an ACE inhibitor or an ARB is a reasonable approach for some individuals.
ACE Inhibitors
| Aceon | perindopril |
| Accupril | quinapril |
| Altace | ramipril |
| Capoten | captopril |
| Lotensin | benazepril |
| Mavik | trandolapril |
| Monopril | fosinopril |
| Prinivil | lisinopril |
| Univasc | moexipril |
| Vasotec | enalapril |
| Zestril | lisinopril |
The ACE Cough
We have been writing about drug-induced coughing for more than 30 years. In the beginning we tried to be diplomatic. Here is one of the first questions we ever received on this topic (March 28, 1988).
Q. Can you recommend a cough remedy I can take for a persistent night-time cough? Most of the brands I have seen caution not to use them if you have high blood pressure. I take Capoten (captopril) to control my blood pressure, so I’m not sure if the warning applies to me.
Here was our answer: You may not need a cough medicine as much as a consultation with your physician. One of the most annoying side effects of captopril (and all ACE inhibitors) can be a dry, hacking cough. It would be a shame to guzzle cough syrup for years trying to control an adverse drug reaction. Your doctor can determine if your medicine is giving you trouble, and if it is, he may consider an alternative medication.
After decades of other questions about ACE inhibitors and coughing, we finally lost our patience. Another question about a lisinopril cough prompted a less tactful response from us.
The Lisinopril Cough from Hell:
Q. I had a severe cough from lisinopril. When it started, I went to my doctor and he sent me to an Ear Nose and Throat Doctor.
The ENT doctor said the cough was from acid reflux and gave me a prescription. No change in my cough.
I had to quit my job because when a coughing spell started up, I had to race to the bathroom and throw up. It interrupted me with customers or on the phone.
I started looking for an explanation online and found out that lisinopril could cause a cough. My doctor said I needed to stay off the internet and that my theory was nonsense.
I decided to go off lisinopril anyway. About a month later, I stopped coughing. My doctor didn’t like my self-diagnosis and put me on a different blood pressure medication. I started coughing again. I need to find a blood pressure med that will not make me cough.
No one gets through medical school without learning about ACE inhibitors and cough. It is probably the most common side effect of such drugs. Doctors should recognize a lisinopril cough and change the blood pressure medication. Arguing with a patient about “self-diagnosis” as the reader above reports, borders on malpractice.
How Common is an ACE inhibitors Cough?
The precise incidence of an ACE inhibitor cough is not known. Reports have it showing up in anywhere from 5% to 35% of patients (Chest Jan. 2006). It can come on within hours of taking the first pill or it can take months or years to reveal itself.
We have lost count of the number of readers who have complained to us about the annoying cough they experience while taking ACEs. One wrote:
“I took lisinopril and developed a cough that would start with a terrible tickle in my throat. Neither cough drops nor syrup had any effect on the problem. I had been taking a generic form of the drug for about the same interval I’d been coughing, and the doctor suggested I go back to the original. But the pharmacist cautioned that both versions contained the same ingredients, so I might not notice any difference. Since I am a singer, I could not take a chance and stopped taking the drug altogether. I will let my doctor know, but in the meantime I continue to exercise, watch my diet, and take my BP regularly. So far no problems.”
For those who have a hard time controlling their blood pressure with diet, exercise and non-drug approaches alone, though, there are other options. More about them shortly.
ACE Angioedema: A Potentially Deadly Reaction!
One of the most frightening side effects of ACE inhibitors is angioedema. Tissues around the face, neck and throat can suddenly begin to swell, and the air passage may become blocked. This complication could be lethal without immediate emergency treatment.
A susceptible person may experience this reaction within a short time of starting on the drug; however, some people have an episode of angioedema months or years after they have been taking an ACE inhibitor without problems. Sometimes the first symptom is numbness in the affected tissues, before the swelling begins. Call 911 at the first signs of angioedema!
An Example Of a Delayed Reaction:
Q. I am a pharmacist and had taken lisinopril for over 12 years before I had an angioedema attack. About 8:00 PM, I started having allergic symptoms. By 10:00 PM, my face was swelling, and I couldn’t talk.
I rushed to the nearest hospital emergency room and was immediately diagnosed with angioedema. They started a steroid IV and about midnight I was on my way to recovery. I was discharged the next morning after being in the ICU overnight.
Despite my pharmacy education, I couldn’t imagine that such a delayed reaction (12 years!) could occur. This must be emphasized during patient counseling.
Angioedema Can Be Deadly!
Doctors may not always warn about the early symptoms of angioedema. And sometimes there is no warning. Patients should always be advised to call 911 in the event of numbness or swelling of the lips, mouth, tongue or throat.
Q. Thank you for writing recently about lisinopril and angioedema. My late husband took lisinopril for over 16 years for high blood pressure. He died suddenly when his throat closed up. Although he had many symptoms leading up to this fatal episode, the doctor did not attribute them to lisinopril. I hope others are saved by the information you shared.
Abdominal Angioedema:
The face is not the only part of the body that can be affected. Hands, genitals and the intestines may also react. When angioedema strikes the digestive tract, it can cause abdominal swelling or distention and in some cases bowel obstruction. We have heard from many patients that this condition can be hard to diagnose. It can also be terrifying. Lauryn described her experience:
“I woke up three weeks ago with swelling on the left side of my face. My bottom lip was very swollen as well as my left eye. I went to the bathroom and noticed all of this. Next I had very strong abdominal pains and as I went to the bathroom I realized I was having diarrhea that would not stop. Soon I realized I was having a lot of blood come out with the diarrhea. I was scared. I knew something was wrong.
“I woke my daughter up who happened to spend the night and I told her something was very wrong. She called 911. They came shortly afterwards and I was on the way to the ER. Right after I got there, I was back on the toilet with blood running out of my bowels. A man came in to take my blood pressure and shortly afterwards I was back in bed. I couldn’t remember how I got back there. The doctors and nurses informed me that I had passed out while on the commode from too much blood loss.
“I ended up staying in the hospital two weeks in ICU. They found out that the medicine lisinopril caused angioedema in my abdomen causing it to burst. The rupture in my small intestines led to the GI bleed. I passed out twice and had to undergo a couple surgeries as well as many blood transfusions because of so much blood loss.
“I’m now home recovering, but I’m so weak still from blood loss. I’m just taking it one day at a time. My PC Doctor said it will take a month to get all my energy back and for me to start back feeling 100%. This was a scary ordeal for me and I pray no one has to go through what I encountered with this medication.”
Another visitor to our website responded:
“The reaction to lisinopril is the worst pain I’ve ever had, worse even than labor. It was ridiculous that they did so many tests and still couldn’t figure it out for so long.
“I know doctors think this is really rare. I had to look up the exact words ‘intestinal angioedema lisinopril’ to find it online. But I think when you get a prescription you should get information on all of the side effects. My doctors were considering removing part of my intestine at one point. If only they had realized sooner that lisinopril was the cause, I wouldn’t have suffered so long.”
Christie reports a lengthy ordeal:
“I had angioedema in my intestine and it took over two and a half months for doctors to figure out that it was the lisinopril because it’s such a rare reaction. They couldn’t believe I didn’t have the swelling in my mouth, throat, etc. as well.
“I wish pharmacies put the rare reactions on the info they give you about drugs but they usually only list the ‘common’ side effects. It’s a long road to recovery. I had two surgeries and spent a month in the hospital because of this medicine.”
Beware Misdiagnosis of Angioedema!
“I was put on lisinopril for high blood pressure. Within a month I experienced severe stomach cramping and vomiting. I was rolling on the floor in agony. The doctor said it was most likely the flu but started me on two different antibiotics in case it was bacterial.
“A few weeks later I had another attack with severe stomach cramping and vomiting. I went to the ER, where I was given IV pain meds. A CT scan showed small intestine inflammation partially blocking off my bowel. I was sent home but returned the next day with pain that was a 10 on a 10-point scale. The doctor said that all the tests had been done and there was nothing he could do. I was sent home with pain medication.
“A few weeks later I was admitted to the hospital with increased small intestine inflammation and another blockage. After vomiting for 12 hours, I was released four days later with no definitive diagnosis.
“The doctors said most likely I had Crohn’s disease, but a subsequent colonoscopy was negative for Crohn’s. I underwent extensive tests, including endoscopy, and all were negative. None of the doctors made a connection with the drug lisinopril.
“After two months of missing work, three more ER visits and untold suffering, I found several other people who reported similar symptoms connected to lisinopril. I stopped the medication and have not had another attack. If you look on PubMed you can see reports on lisinopril and intestinal angioedema, but doctors don’t think to connect this with lisinopril because it is not listed as a common side effect.”
Our bottom line on ACE inhibitors:
- Many people tolerate this class of medicines without problems. If your doctor prescribes a drug like lisinopril and you do not develop a cough or angioedema, great!
- At the first signs of a cough, nausea, vomiting, bloating, cramping or abdominal pain, let your doctor know that you are suffering and it might be related to an ACE inhibitor.
- Numbness of the lips, mouth, tongue or throat could be early warning signs of angioedema! Call 911 and/or go immediately to the nearest emergency department. Do not wait for swelling to show up!
Angiotensin Receptor Blockers
| Atacand | candesartan |
| Avapro | irbesartan |
| Benicar | olmesartan |
| Cozaar | losartan |
| Diovan | valsartan |
| Hyzaar | losartan + HCTZ |
| Micardis | telmisartan |
| Teveten | eprosartan |
Angiotensin receptor blockers, or ARBs, work in a way somewhat similar to ACE inhibitors. Rather than blocking the angiotensin-converting enzyme, however, they block the receptor for angiotensin II. They’re less likely to cause the persistant, nagging cough that can be associated with ACEs, though, so they may be a good alternative for people who can’t tolerate ACEs.
Are ARBs as good as ACEs at controlling high blood pressure? The answer seems to be yes. Some cardiologists are now prescribing ACEs and ARBs in combination for maximum blood-pressure lowering benefits. One issue that you may want to discuss with your physician, however, is that there is still some question about whether or not ARBs are as effective at preventing heart attacks as ACEs. As with ACE inhibtors, pregnant women must avoid these medications.
Side Effects:
Adverse reactions are rare but may include stomach upset, muscle cramps, and dizziness. Dry mouth and dry skin are not unusual, and some patients report dry eyes. Cough is not as common as with the ACE inhibitors, but it can occur. Headache, digestive distress, joint pain, hair loss and kidney or liver damage may occur. Again, as with ACE inhibitors, angioedema is a serious side effect that requires emergency medical attention. ARBs can lead to potassium buildup (hyperkalemia). These drugs are not appropriate for pregnant women, as they are toxic to the fetus.
ARBs and Suicide:
One possible side effect that can be very serious is a greater risk of suicide (JAMA Network Open, Oct. 16, 2019). Canadian researchers have found that people taking ARBs are more likely to commit suicide than those on ACE inhibitors or other blood pressure medicines. An editorial notes that angiotensin can affect brain activity and possibly mood. It suggests clinicians consider ACE inhibitors rather than ARBs, especially for patients who may be at risk of depression.
Interactions:
Cozaar interacts with cimetidine (Tagamet) and barbiturates. In general, ARBs should not be used in combination with other potassium-sparing drugs. As with ACE inhibitors, this includes the antibiotic cotrimoxazole (Bactrim, Septra, TMP-SMZ). People using an ARB should never also take aliskiren. This combination could also greatly increase the risk of hyperkalemia (excess potassium).
Aliskiren
Technically, we should have titled this section direct renin inhbitors. However, at this time, there is only one drug in its class: aliskiren (Tekturna). As with ACE inhibitors and ARBs, aliskiren works through its actions on the renin-angiotensin system. LIke those other categories of drugs, aliskiren is not appropriate during pregnancy and should be discontinued as soon as a woman realizes she is pregnant.
Although aliskiren lowers blood pressure more than other antihypertensive drugs, it does not appear to keep people from dying prematurely (Journal of Human Hypertension, Nov. 2019). Its use for treating people with diabetes is still controversial.
Side Effects:
People taking this drug may experience diarrhea, which is the most common side effect. Others include cough, chills, headache, nasal congestion, sore throat or unusual fatigue . Aliskiren can affect the kidneys; the most common sign of this is an elevated BUN or creatine level. The medication can increase potassium levels on its own or in comibination with other potassium-sparing medications. Angioedema and very serious skin reactions (Stevens-Johnson syndrome and toxic epidermal necrolysis) deserve emergency attention.
Interactions:
Aliskiren should not be taken with any ARB or ACE inhibitor. It may lower blood levels of furosemide (Lasix) and may interact with cyclosporine, itraconazole, amiodarone, clarithromycin or erythromycin.
Calcium Channel Blockers
| Adalat | nifedipine |
| Calan | verapamil |
| Cardene | nicardipine |
| Cardizem | diltiazem |
| Covera-HS | verapamil |
| Dilacor XR | diltiazem |
| DynaCirc | isradipine |
| Isoptin | verapamil |
| Norvasc | amlodipine |
| Plendil | felodipine |
| Procardia | nifedipine |
| Sular | nisoldipine |
| Tiazac | diltiazem |
| Vascor | bepridil |
| Verelan | verapamil |
Calcium channel blockers became popular in the 1980s because they appeared to have fewer side effects than previous drugs. Not only did they control angina and blood pressure, they offered relief for a variety of other problems including certain arrhythmias, migraines, strokes, and Raynaud’s syndrome.
There are now data to suggest, however, that their safety may be in question. Instead of a clear indication that calcium antagonists improve and prolong life, there is concern that some of these medications may actually predispose certain people to heart attacks and increase the risk of heart failure.
Clearly there are specific situations in which drugs like Norvasc, Calan, Cardizem, Covera-HS, Isoptin and Verelan may be necessary. And of course no one should ever stop any medication without medical supervision. But be sure to discuss all potential risks and side effects of your medications with your physician.
Cautions:
Older people may be vulnerable to dizziness if they stand suddenly. Severe heart conditions or kidney or liver disease may create special problems for people on these medicines.
Side Effects:
Nifedipine can produce flushing, dizziness, headache, nausea and fluid retention (swollen ankles or hands). Other adverse effects may include irregular heart beats, breathing difficulties, trouble sleeping or sexual problems. Verapamil can cause constipation, hair loss, dizziness, swollen hands or feet, sexual difficulties, headache or rash. Diltiazem is often well tolerated, but some people experience fluid retention, dizziness, headache or flushing. Other reactions include nausea, constipation, sensitivity to sunburn and rash. Amlodipine may produce rash, dizziness, headache, weakness, upset stomach, swollen gums, fatigue and fluid retention.
Interactions:
People with heart rhythm problems may be prescribed quinidine, which may be dangerous in combination with nifedipine or verapamil. When a beta blocker is combined with a calcium antagonist, cardiac function should be monitored carefully. Certain calcium blockers may also interact with antidepressants, barbiturates, carbamazepine (Tegretol), cimetidine (Tagamet), cyclosporine (Sandimmune), digoxin (Lanoxin), grapefruit juice and theophylline.
Beta Blockers
| Blocadren | timolol |
| Cartrol | carteolol |
| Corgard | nadolol |
| Inderal | propranolol |
| Kerlone | betaxolol |
| Levatol | penbutolol |
| Lopressor | metoprolol |
| Sectral | acebutolol |
| Tenormin | atenolol |
| Toprol XL | metoprolol |
| Visken | pindolol |
| Zebeta | bisoprolol |
Beta blockers are some of the most widely prescribed blood pressure drugs; more than 115 million prescriptions are dispensed for them annually, with atenolol and metoprolol at the helm. They’re also used to control angina, normalize irregular heart rhythms, lower the risk of repeat heart attacks, prevent migraines and diminish performance anxiety.
They vary widely in their side effect and interaction profiles, but we now have fairly grave concerns about some of their hazards. We would not recommend these drugs as the first or even second line of defense for controlling high blood pressure. They’re simply not as effective as they should be, particularly atenolol.
There are many beta blockers, so what follows is general information. For more details on a specific drug, please check with your physician and pharmacist.
Cautions:
People who have asthma and other serious breathing problems can get into terrible trouble with many beta blockers, as these drugs can lead to constricted airways. Diabetes and thyroid disorders may also be harder to treat. Never stop a beta blocker suddenly, since this could trigger angina, irregular heart rhythms or even a heart attack.
Side Effects:
Some effects associated with drugs like propranolol include slow heart rate, cold hands and feet, fatigue, stomach upset, insomnia, nightmares, shortness of breath, rash, hair loss, blurred vision, dizziness, joint pain and sexual difficulties. Some people experience the “beta blocker blues”: depression, nightmares, confusion, memory problems, and lethargy. Cholesterol elevation may also occur with certain beta blockers, so blood tests are recommended.
Beta-Blocker Blues:
Beware of the beta-blocker blues. When one of our readers was prescribed beta blockers, he reported:
“I went through a living hell because I became severely depressed. When I complained [to my doctor] of my depressed feelings and asked if the medication might be responsible, he brushed my concerns aside and prescribed an antidepressant. It made me anxious and gave me insomnia, so he added a tranquilizer.”
Interactions:
Other blood pressure pills may be prescribed in combination with beta blockers. If clonidine (Catapres) is stopped suddenly in such a situation, blood pressure may rise to life-threatening levels. No one should ever stop clonidine without medical supervision!
NSAIDs may reduce beta-blockers’ effectiveness. Other medications that may interact with beta blockers include ampicillin, anti-psychotics, barbiturates, cimetidine, ergotamine, oral contraceptives, rifampin, theophylline and some drugs for irregular heart rhythms (amiodarone, flecainide, propafenone, quinidine).
It should be possible to control blood pressure without experiencing unpleasant side effects. Anyone taking a diuretic such as hydrochlorothiazide should monitor mineral levels like potassium or magnesium.
What Happens When Nothing Works Well?
You would think that with all the options listed above that everyone would be able to access a blood pressure treatment that controls hypertension without unpleasant side effects. You would be wrong! That’s because every single medication that was listed above can cause some side effects for some people.
For example, diuretics such as hydrochlorothiazide will often deplete minerals like potassium, magnesium and zinc. Although potassium is frequently monitored with blood tests, magnesium and zinc may go ignored. That can lead to all sorts of mischief. And let’s not forget sun sensitivity. We mentioned “increased susceptibility to sunburn.” But that’s only part of the problem. Thiazide diuretics can increase the risk for skin cancer. You can read more about that serious problem at this link.
Ace inhibitors (ACEis) such as lisinopril can cause the infamous cough or angioedema. These complications can be disastrous. Angiotensin receptor blockers (ARBs) like losartan or valsartan are less likely to cause a cough, but it is not out of the question. Some people complain of dizziness, digestive distress and dry mouth.
Doctors often turn to calcium channel blockers such as nifedipine if the above drugs are problematic. But side effects such as dizziness, headache, swollen ankles and sleeping problems can make calcium antagonists difficult. Finally, beta blockers such a metoprolol can slow the heart rate dramatically depending upon the dose. Some patients complain of the beta blocker blahs. There are also sexual difficulties, depression and fatigue to contend with.
When all else fails or doesn’t do the job, what else is available? There is a relatively new medication called Tryvio (aprocitentan). It was approved by the FDA in March of 2024. The drug got a green light from the agency:
“in combination with other antihypertensive drugs…in patients who are not adequately controlled on other drugs.”
Endothelin-Receptor Antagonist:
Tryvio (aprocitentan) is the first of a new class of blood pressure meds. It is clearly not a first-line medication. That’s partly because the FDA has made clear that it is only supposed to be prescribed when blood pressure is not adequately controlled with more traditional medicines. It is also supposed to be taken in combination with some other antihypertensive drug.
Then there’s the price. Most BP drugs have been on the market so long that they are available in generic formulations that are quite inexpensive. Tryvio is only available as a brand name BP drug. GoodRx lists it at the time of this writing at over $900 for a month’s supply. With a coupon, it is still over $800. Some insurance companies may balk at that price, especially since a month’s worth of lisinopril is often less than $15.
Cautions:
The biggest problem with aprocitentan is birth defects. Patients who might become pregnant must obtain two negative pregnancy tests before they can even contemplate taking Tryvio. Then they “should use acceptable methods of contraception before the start of, during, and for one month after stopping treatment.”
Because of the risk of birth defects:
- Prescribers must be certified with the TRYVIO REMS [Risk Evaluation and Mitigation Strategy] by enrolling and completing training.
- Pharmacies that dispense TRYVIO must be certified with the TRYVIO REMS.
Other serious cautions about Tryvio have to do with liver toxicity. Anyone with a history of hepatotoxicity needs to evaluated before starting treatment. And if symptoms of liver damage occur “(nausea, vomiting, right upper quadrant pain, fatigue, anorexia, scleral icterus, jaundice, dark urine, fever, or itching)” the drug needs to be stopped immediately!
If there is fluid retention (edema), that could be a red flag. Patients should also be monitored for a decrease in hemoglobin levels.
Side Effects:
Two adverse reactions to be aware of are fluid retention and anemia. Sperm counts may also go down. Although relatively rare, patients should be on the lookout for any allergic reactions such as rash.
Interactions:
The official prescribing information for Tryvio does not list any specific drug interactions. There is one drug, isocarboxazid (Marplan) that must be avoided. Other drugs that should not be combined with Tryvio include adesleukin (Proleukin) and aripiprazole (Abilify). Always check with the prescribing physician and pharmacist, though, to make sure there are not other meds that are incompatible with Tryvio.
Final Words:
There are a lot of options when it comes to controlling blood pressure. We obviously favor lifestyle management whenever possible. There are also a number of nondrug options that we have listed in this eGuide. When such strategies are ineffective, though, medications can make a difference.
There is no one medicine that works well for everyone. Many people tolerate ACE inhibitors or ARBs without complications. Others find that a diuretic like HCTZ does the job. No one should live with dizziness or brain fog or an unremitting cough. If one medicine causes symptoms, trial and error should eventually lead to something that works well. Please let us know what does the job for you by adding your comment to one of the blood pressure articles on our website: www.PeoplesPharmacy.com.
Publication Information
Published on: July 22, 2024
|
Last Updated: November 23, 2024
Publisher: The People's Pharmacy
© 2026 The People's Pharmacy
