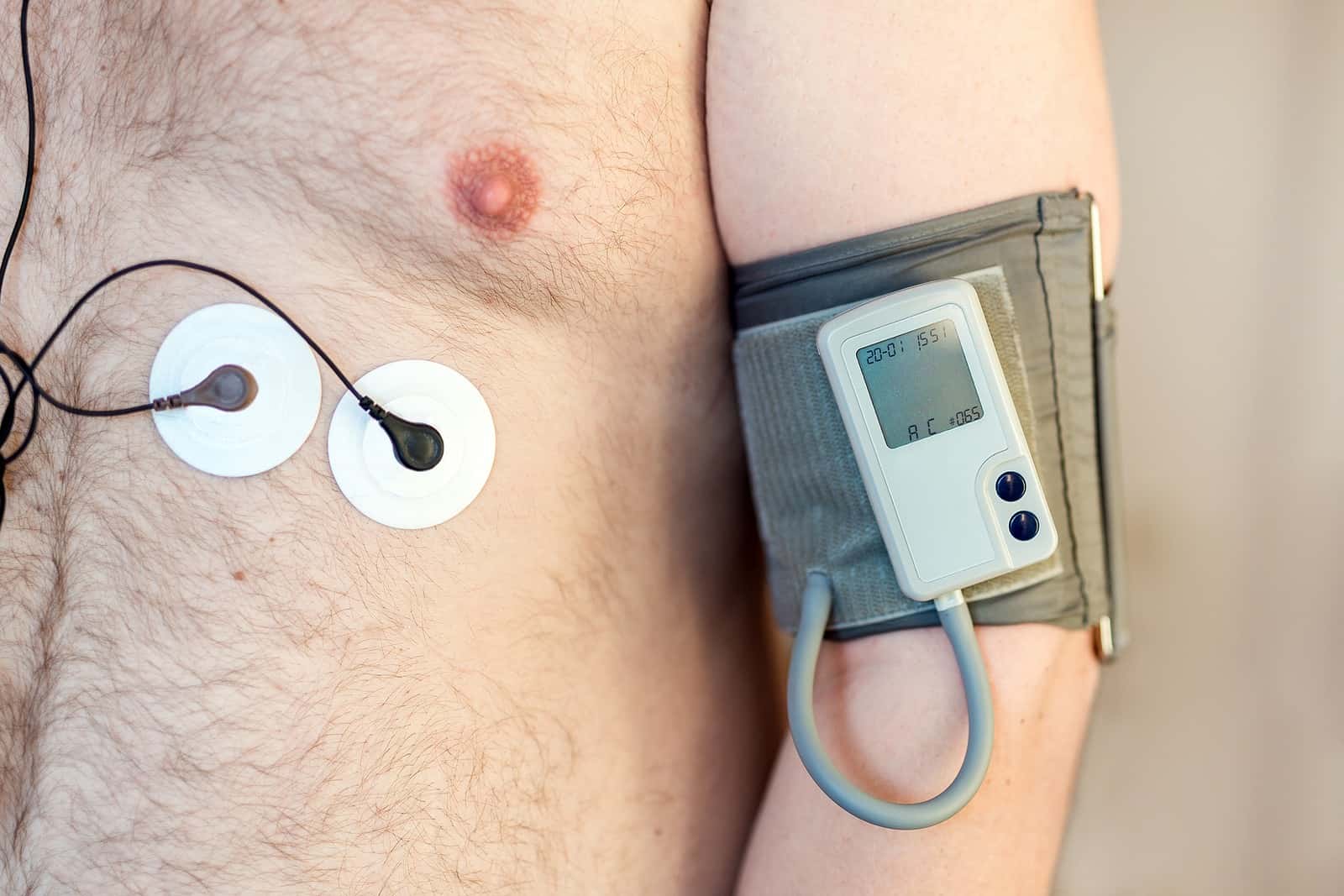
Health professionals often rely upon blood pressure measurements taken in the clinic to diagnose hypertension. If a patient has a blood pressure (BP) reading greater than 120/80 in a doctor’s office, it would be labeled “elevated.” That’s thanks to guidelines from the American Heart Association andAmerican College of Cardiology. To be considered “normal” you have to be lower than 120/80. Over 120 million Americans are now classified as hypertensive. But what’s the most reliable predictor of heart attacks or death from hypertension: blood pressure measurements taken in the doctor’s office or at home over 24 hours or several days? (The photo at the top of the page shows a Holter monitor for heart rhythms plus an ambulatory blood pressure [ABP] monitor for continuous BP readings throughout the day and night.)
Why Blood Pressure Measurements Ignore Real Life
A reader recently took us to task for complaining about the way healthcare professionals measure blood pressure in the doctor’s office:
Q. You have repeatedly criticized healthcare workers for making mistakes when measuring blood pressure. No one has answered my question of why a “proper” blood pressure reading requires me to assume a state that I exist in perhaps one percent of the time during an average day. That is, sitting in a chair, feet flat on the floor, arm level with my heart on an arm rest, empty bladder and perfectly quiet for five minutes.
If I wanted to know what my blood pressure is 99 percent of the time during a typical day, it should be measured while in that typical state. That is walking, talking, typing, etc. I don’t understand why you are so stubborn about BP measuring technique.
A. You make a very good point. Blood pressure fluctuates constantly throughout the day. Stress, physical activity, driving, reading, talking, or even watching television can all raise or lower blood pressure. So which number reflects your actual blood pressure?
The honest answer is: no single reading does.
To capture a realistic picture, you would need to wear a portable device for a full day, or two, or seven. This ambulatory blood pressure monitor automatically checks BP every 15 to 30 minutes during the day and every 30 to 60 minutes while you sleep. With that information, a physician can calculate your average blood pressure over time. Blood pressure while you sleep turns out to be important.
Blood Pressure Measurements Put to the Test: The Flawed Spanish Study
Which blood pressure measurements best predict heart attacks, strokes, or death—those taken in the doctor’s office, or those recorded repeatedly during everyday life?
To answer that question, researchers in Spain conducted an interesting study. The New England Journal of Medicine (April 19, 2018) reported the results. The investigators followed nearly 64,000 patients from 2004 to 2014.
Each participant had:
- Clinic blood pressure measurements, taken according to standard protocols
- 24-hour ambulatory blood pressure measurements, recorded every 20 minutes during the day and every 30 minutes at night
The researchers then tracked deaths over a median follow-up of 4.7 years.
By the end of the study:
- 3,808 people had died
- 1,295 deaths were due to cardiovascular causes
Which Blood Pressure Measurements Predicted Death?
Hypertension was defined as:
- Clinic readings: ≥140 systolic or ≥90 diastolic
- Ambulatory readings: ≥130 systolic or ≥80 diastolic
And yes, Spanish physicians back in those days defined hypertension quite differently than American physicians do today.
The key question:
Which blood pressure measurements best predicted mortality?
What was the best predictor of death: blood pressure measurements taken in the doctor’s office or at home with a 24-hour recording device (ambulatory readings)?
Ambulatory Blood Pressure Measurements Win!
An editorial in the New England Journal of Medicine (April 19, 2018) that accompanied the research described the results this way:
“They observed that ambulatory blood-pressure measurements were a stronger predictor of all-cause and cardiovascular mortality than clinic blood-pressure values.”
That all sounds fine and dandy…but the original article was “retracted.” The authors wrote on January 29, 2020:
“Because we have identified inaccuracies in the analytic database and data analyses underlying ‘Relationship between Clinic and Ambulatory Blood-Pressure Measurements and Mortality,’ which was published in the April 19, 2018, issue of the Journal we wish to retract the article.”
It is never good news when authors have to retract their research. Because we hate to leave this critical question in limbo, we went looking for newer research. We found an article in JAMA (Aug. 6, 2019). It was titled: “Association of Office and Ambulatory Blood Pressure With Mortality and Cardiovascular Outcomes.”
The researchers recruited 11,395 participants and tracked them over a median of 13.8 years. And the envelope please:
“In this population-based cohort study, higher 24-hour and nighttime BP were significantly associated with greater risks of death and a composite cardiovascular outcome, even after adjusting for other office-based or ambulatory blood pressure measurements.
“Over the past 30 years, ambulatory BP monitoring developed into the recommended technique for BP measurement. The current population-based study confirmed previous research, indicating that ambulatory BP monitoring over and beyond measures taken in clinicians’ offices improved risk stratification among patients with or those suspected of having hypertension. It strengthened the notion that nighttime BP measures carry valuable prognostic information.”
That’s a lot of doctorspeak. The bottom line is that 24-hour automatic BP readings were better predictors than office readings. A Review of 14,230 individuals in 14 population cohorts was published in the European Heart Journal (April 18, 2025).
The authors noted:
“Numerous studies reported that total and cause-specific mortality and fatal combined with non-fatal cardiovascular complications are associated with the ABP [ambulatory blood pressure] level and that these associations were stronger for ABP and home BP than for OBP [office blood pressure].”
These researchers conclude that office blood pressure readings often misclassify individuals with regard to BP control and that continuous monitoring with ABP or home blood pressure measurement is necessary to verify what’s really going on.
If Your Life Were a Book…
Think of your life as a very large book.
A single office visit—one blood pressure measurement taken under artificial conditions—is like reading one sentence and trying to understand the entire story.
A 24-hour ambulatory monitor? That’s one page.
Better than a sentence, but still incomplete.
The most meaningful approach is to collect many blood pressure measurements over weeks, months, and years—at home, at work, at different times of day, under real-life conditions. When you log those numbers in a notebook or spreadsheet, patterns emerge.
That long view—the story, not the snapshot—is what truly reflects your cardiovascular risk.
Blood Pressure Measurements at Home: Technique Matters
One of the biggest obstacles to reliable blood pressure measurements is poor technique. We have watched countless readings taken incorrectly in clinics: legs crossed, arms dangling, rushed procedures, no rest period.
These errors can raise systolic blood pressure by 10 to 20 points, enough to trigger unnecessary treatment.
We detail the most common mistakes—and how to fix them—here:
What’s the Best Way to Measure Blood Pressure?
What’s better, blood pressure readings at the doctor’s office or at home? A new study will surprise many health professionals. BP strategies!
That article also reveals the most reliable blood pressure monitoring devices.
One Reader’s Real-Life Experience With Blood Pressure Measurements
Steve in Maryland is an engaged patient. Here is his story:
“Thank you very much for this article. I have been measuring my BP at home for 5 years. I keep the readings on a spread sheet. I’m 65 years old and take 10 mg of lisinopril. During a recent visit to my primary care doctor my blood pressure was once again measured incorrectly. It always is, and my readings are always higher than at home.
“When my doctor visited with me for 5 minutes he pulled up my chart on his iPad and told me that we needed to do more about my BP as it was borderline the last three visits. I shared with him my concern about the conflict between his data and mine. Remember, I have been measuring mine for 5 years. My data includes all seasons, time of day and every other influence.
“He pointed to his iPad and said here are the numbers. They don’t lie. I said yes, but I think mine carry more importance as there is more data and a broader sample. He stood firm on his information and had no interest in what I had to say. The conversation ended.
“When I first entered his practice many years ago I told him I am actively involved in my care. If exercise and diet help, I do it. If herbs or supplements help, I take them. If no other option exists other than a pharmaceutical, I take it. So, I ask questions and make my own decisions about the path I will follow. I don’t think he appreciates my level of knowledge and involvement.
“I don’t think it’s just him. Our medical care system is weighted toward what I call ‘check box medicine’ and drugs. Check box means you show up, they go through a number of preprogrammed steps and out the door you go with a drug or follow-up appointment. We can thank insurance companies, lawyers, bureaucrats and many others.
“In my book, nothing will change unless we the people learn to be the most important part of our care.”
Five years of real-world blood pressure measurements across seasons, times of day, and daily stresses tell a far richer story than three rushed clinic readings.
The People’s Pharmacy Perspective on Blood Pressure Measurements
We believe patients should be active partners in their care—not passive recipients of numbers generated by hurried systems.
Blood pressure measurements matter enormously. But how, when, and where they are taken matters just as much.
If you’d like to dig deeper, our eGuide to Blood Pressure Solutions offers practical, evidence-based strategies for understanding your numbers and working effectively with your healthcare provider. It can be found under the Health eGuides tab. You will also find BP devices that pass muster.
Join the Conversation
Have your blood pressure measurements told conflicting stories? Share your experience in the comments below—you’re not alone. We would love it if you would share this report with friends and family. Chances are very good that some people you know have elevated blood pressure readings. They might appreciate this article more than you imagine. While you are at it, please encourage them to sign up for our free newsletter. Each new subscription helps keep our newsletter, website, radio shows and podcasts moving forward. Here is a link to subscribe or donate. Thank you for your support.
Citations
- Jones, D.W., et al, "2025 AHA/ACC/AANP/AAPA/ABC/ACCP/ACPM/AGS/AMA/ASPC/NMA/PCNA/SGIM Guideline for the Prevention, Detection, Evaluation and Management of High Blood Pressure in Adults: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines," Hypertension, Dec. 2025, doi: 10.1161/HYP.0000000000000257
- Yang, W-Y., et al, "Association of Office and Ambulatory Blood Pressure With Mortality and Cardiovascular Outcomes," JAMA, Aug. 6, 2019, doi: 10.1001/jama.2019.9811
- Zhang, D-Y, et al, "Ambulatory blood pressure monitoring, European guideline targets, and cardiovascular outcomes: an individual patient data meta-analysis," European Heart Journal, April 18, 2025, doi: 10.1093/eurheartj/ehaf220

