In the 19th century, nobody wanted to go to the hospital. Before antibiotics were discovered, people considered these institutions as the very last resort. The wards were unfriendly and frequently contaminated. Many people perceived the hospital as a place you went to die.
Nowadays, hospitals are often inviting. Many offer private rooms, and in some facilities a family member can spend the night. Hygiene practices have improved significantly.
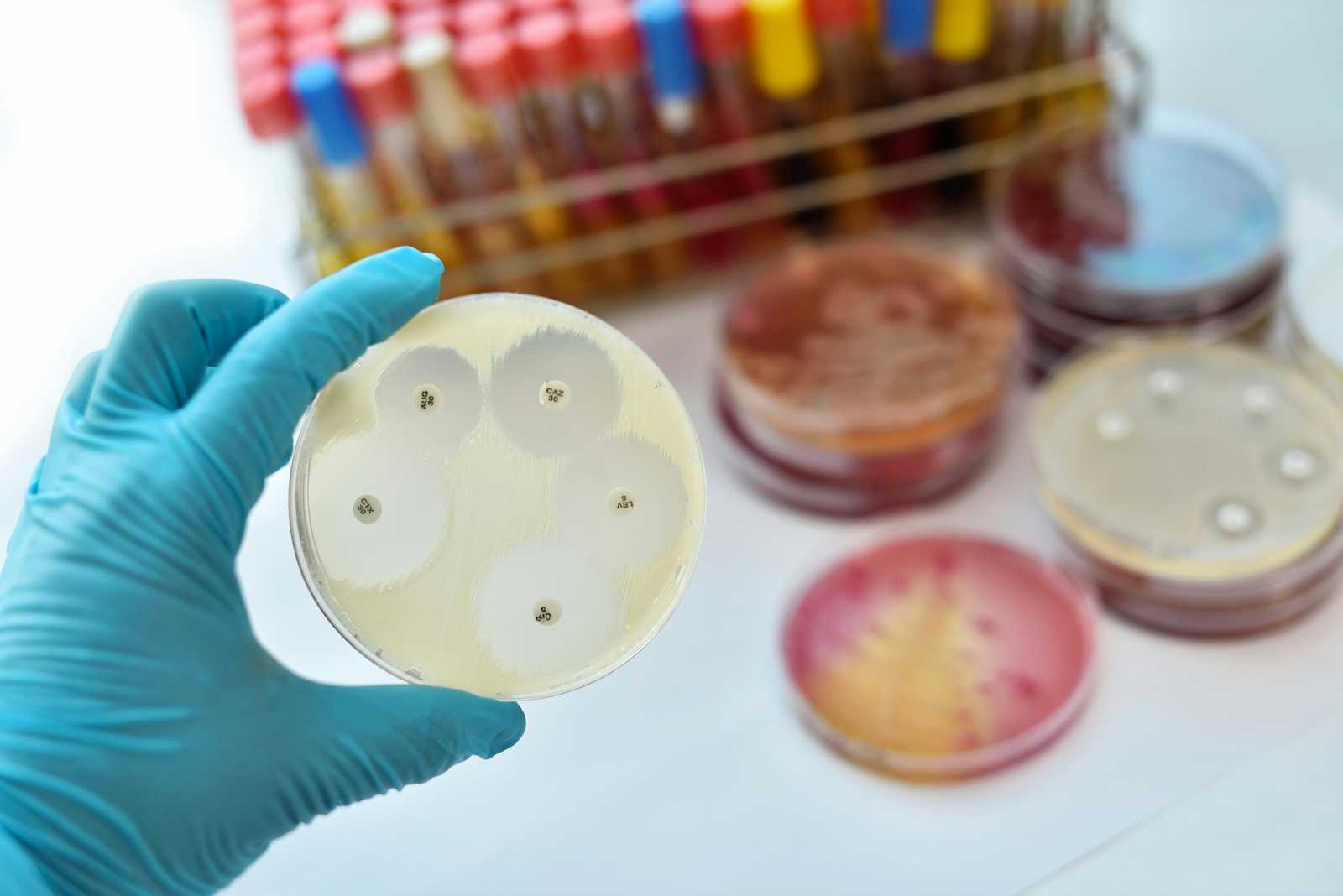
For decades, cleaning strategies and modern antibiotics kept infections under control. Now, however, many pathogens have evolved to resist antimicrobial drugs. We are also learning that these drug-resistant germs may persist in unexpected nooks and crannies of the hospital room and its equipment.
Where Do Drug-Resistant Germs Hide?
Many rooms have privacy curtains, for example. These floor-to-ceiling textiles shield patients from view during procedures. However, the fabric can easily become contaminated with germs. Some microbes have developed resistance to the most frequently used antibiotics and thus pose a health hazard. These data are being presented at the European Congress of Clinical Microbiology and Infectious Diseases in Amsterdam.
Why are there microbes on the curtains? People touch the panels frequently. Doctors and nurses pull them aside or close them. Patients and visitors do the same. And hospitals have not developed clear guidelines on how to clean them to remove any drug-resistant germs.
Fungicide-Resistant Candida:
Bacteria like MRSA (methicillin-resistant Staphylococcus aureus) are not the only hazard lurking in hospital rooms. Epidemiologists have just raised the alarm about a species of fungus that has acquired resistance to multiple anti-fungal drugs. The organism, Candida auris, has caused nearly 600 serious infections in the US. In at least one case, fungal spores were so pervasive and persistent that the hospital had to remove ceiling and floor tiles and all the equipment in the room to get rid of them. Even the mattress was contaminated and presumably needed to be destroyed.
What Britain Does to Fight Drug-Resistant Germs:
In Britain, the National Health Service instituted several policies designed to reduce germ transmission. They include prohibitions on health care workers wearing any jewelry, including watches. Scrubs must leave arms bare below the elbows. Ties and white coats are banned.
Doctors hated the new policies. But over time health professionals throughout the UK have adapted to the requirements.
All these rules raised a lot of eyebrows in the US when they were initiated in the UK in 2008. Infectious disease experts argued that no cases of infection transmission had been unequivocally linked to neckties, white coats, watches or stethoscopes. They cited the lack of clear evidence of transmission to explain that such infection control policies were unnecessary.
Despite this, research has demonstrated that such surfaces are frequently contaminated with a variety of pathogens. So are items such as computer keyboards, tablets, mobile phones, soap dispensers, electrocardiogram leads and nebulizers (Clinical Infectious Diseases, Oct. 15, 2017).
Experts still entertain serious doubts about the importance of any of these contaminated items as sources of infection. After all, health care systems are often secretive about their infection rates and pathogen control measures.
Should the US Follow Britain’s Lead?
Nonetheless, with drug resistant germs becoming increasingly common, health care facilities may wish to pay more attention to infection control procedures. Perhaps US hospitals should consider following UK policies.
Citations
- Kanamori et al, "The role of patient care items as a fomite in healthcare-associated outbreaks and infection prevention." Clinical Infectious Diseases, Oct. 15, 2017. DOI: 10.1093/cid/cix462