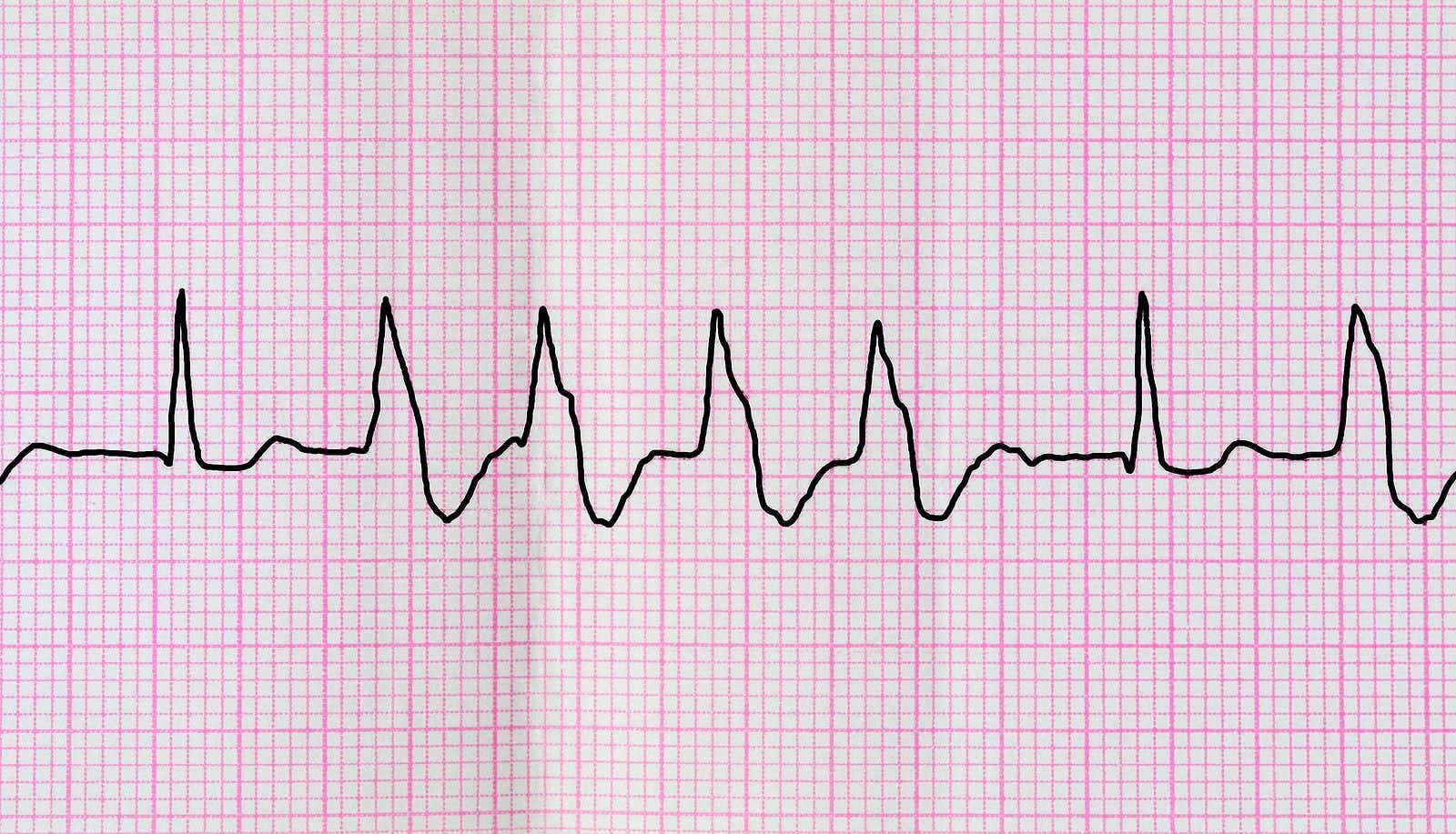
Have you ever looked at your electrocardiogram (ECG)? Do you know if it is normal or if you have an irregular heart rhythm (arrhythmia)? Most engaged patients know about their cholesterol, their blood pressure and maybe even their pulse. But heart rhythm remains mysterious. Not knowing, though, could be deadly.
Drugs and Deadly Arrhythmias:
If someone dies unexpectedly, especially if she is young and healthy, most people chalk it up to a horrible twist of fate. But sometimes such a death might have been prevented.
We first learned of drug-induced heart rhythm disturbances 30 years ago when a reader of our syndicated newspaper column shared this concern about an antihistamine called terfenadine (Seldane).
The letter said:
“I have been taking Seldane for three years for allergies in the spring and fall. I am 54 years old and recently applied for a life insurance policy.
“The company required an ECG, which showed heart rhythm irregularities. All my previous electrocardiograms were normal and there is no family history of heart problems.
“I was very interested in your recent article suggesting that Seldane might cause heart rhythm changes. I would hate to be turned down for insurance because of a drug reaction.”
We advised this person to consider another antihistamine for her allergies. There were whispers that terfenadine might cause arrhythmias in susceptible individuals.
Seldane Interactions and Arrhythmias:
Another reader shared this story:
“My wife loves grapefruit, and usually eats it every day. Last fall she was taking Seldane for her allergies and had to take medicine for a yeast infection. She had a number of dizzy spells and even fainted once, but her doctors couldn’t figure out what was wrong. Now that allergy season is over, she feels fine.”
Our answer:
Thank goodness she survived! Either the antifungal drug for her vaginal yeast infection or her morning grapefruit could have pushed her Seldane dose too high. The dizziness and fainting might be the first symptoms of a heart rhythm disturbance. Grapefruit can be dangerous when combined with certain other medications.
The FDA knows of 40 cases of serious heart rhythm disturbances and at least eight deaths associated with Seldane. For this reason the feds want Seldane to disappear from pharmacy shelves.
Death by Grapefruit and Seldane:
Before the Food and Drug Administration could require the makers of Seldane to recall this antihistamine we received this tragic story:
A young man was in good health except for allergies. His physician prescribed Seldane. This patient liked grapefruit juice and drank it several times a week. Neither his wife nor young daughter liked or drank it.
The day he died, he consumed two glasses of grapefruit juice as well as his medicine. The cause of death was determined to be “terfenadine intoxication,” even though he had taken his prescribed dose. His blood levels of Seldane were as high as those seen in other people who experienced fatal irregular heart rhythms due to Seldane overdose.
A grieving grandparent shared this story:
“Our 19-year-old granddaughter died in her sleep while she was at college. She had taken Seldane and it caused violent heart arrhythmias.”
Eventually the FDA did encourage the removal of Seldane and another nonsedating antihistamine called astemizole (Hismanal). These medications could impact the heart by themselves. When combined with antifungal medications, antibiotics like azithromycin and erythromycin or certain antidepressants the risk of arrhythmias was increased.
Why Should You Care About Heart Rhythm Abnormalities?
Two of the most controversial drugs we have written about in recent memory involve the malarial drug hydroxychloroquine (HCQ) and the antibiotic azithromycin. These drugs have been held out as game changers for treating the coronavirus.
The final word on hydroxychloroquine (HCQ) and azithromycin against the coronavirus is not yet in. We remain hopeful that randomized controlled trials may reveal benefits either as a preventive against COVID-19 or in speeding healing. But there is now ample evidence that each drug alone and both drugs together can increase the risk for dangerous heart rhythm disturbances.
One study demonstrating that was published in The Lancet (May 22, 2020). More than 96,000 COVID-19 positive patients from 671 hospitals participated. Nearly 15,000 received drug treatment with either hydroxychloroquine or chloroquine. These compounds have long been used against malaria and have been pressed into service on the possibility they might help fight the SARS-CoV-2 virus that causes COVID-19.
The investigators analyzed patients’ medical records. This type of retrospective scrutiny is considered an observational study. It isn’t as strong as an actual experiment in which volunteers are randomly assigned to treatment or placebo.
Still, with information on so many people, scientists are alarmed to find that the drugs did not appear to help people recover more quickly or survive longer. On the contrary, people taking one of these drugs were more likely to develop heart rhythm problems that can lead to premature death.
Doctors have long known about the potential for chloroquine and hydroxychloroquine to disrupt heart rhythm. That is one reason the FDA has warned people not to take hydroxychloroquine except as part of a clinical trial. This way they can receive an electrocardiogram in advance of treatment.
Even more worrisome, many people taking one of the malaria drugs also took an antibiotic called azithromycin at the same time. This medicine, also called Z-Pak, was hypothesized to work together with the chloroquine-type medicines against the virus.
HCQ + Z-Pak Increased the Risk for Arrhythmias:
People taking HCQ alone were 137 percent more likely to experience a dangerous heart arrhythmia. If they took the malaria drug together with azithromycin, the increased risk of a serious heart rhythm abnormality was more than 400 percent.
Are You Taking A Drug That Disrupts Heart Rhythm?
We hope that all this attention to heart arrhythmias triggered by hydroxychloroquine and azithromycin will remind health care professionals that there are over 100 other medications that can also alter heart rhythms.
Remember, that is why the FDA encouraged the removal of the antihistamines Seldane and Hismanal. They too could interact with drugs like azithromycin to prolong the QT interval on an electrocardiogram (ECG). This is also what happened to some COVID-19 patients who were taking both azithromycin and HCQ together.
Readers Infuriated About Reports of Hydroxychloroquine and Azithromycin Arrhythmias:
We have been surprised by the anger many of our readers have expressed that we would write about irregular heart rhythms associated with both HCQ and azithromycin. Here is just one example:
John complains that we have not been fair:
“Why hasn’t People’s Pharmacy and the media urged lupus and arthritis users to stop using hydroxychloroquine if it is so dangerous?”
Our answer to John:
“There is no doubt that HCQ works for lupus and rheumatoid arthritis. The drug has FDA approval for these indications.
“We would certainly hope that any physician who plans to prescribe HCQ to patients with these conditions would order an ECG beforehand to make sure the patient does not have long QT interval or another condition called G6PD deficiency!”
OK, we bet you have never heard of G6PD deficiency. But it’s important. You can read about this fascinating metabolic condition and learn how to interpret your own ECG at this link.
Robin says that criticism of HCQ is not credible:
“People have been treated with hydroxychloroquine for lupus and RA for many decades, without any major or serious side effects. Why would harm to the heart suddenly become a major side effect for only those with covid-19? Not credible.
“Many MDs around the US and in other countries have been treating COVID-19 patients with this drug with significant positive results and virtually no serious side effects.”
People’s Pharmacy Perspective
As stated above, we would certainly hope that any patient treated with HCQ or azithromycin would get an electrocardiogram first to rule out a long QT interval. We wouldn’t be so sure that patients with RA or lupus have never been harmed by HCQ. If someone dies while taking such a medicine, will the doctor recognize the cause was a fatal arrhythmia or just chalk it up to bad luck?
The French scientist who has administered the combination of HCQ and azithromycin to COVID-19 patients is reported to have ordered ECGs before administering such drugs. That seems reasonable to us. The bottom line seems to be that if a person does not have a long QT interval, the cardiac risks are manageable, as long as there is clear evidence that the drugs actually work.
We certainly hope that hydroxychloroquine is proven effective either as a preventive medicine or as a treatment against COVID-19. Until we have proof, however, we urge caution. An ECG is critical to rule out long QT interval and susceptibility to life-threatening arrhythmias.
Other Drugs That Cause Long QT Interval:
Now that physicians have become acutely aware of the consequences of drug-induced heart-rhythm problems, they must monitor patients who are taking such medicines. Better yet, they should order an ECG and ask the cardiologist to check for long QT interval or an arrhythmia called torsades de pointes. Here is just a partial list of drugs that could be problematic:
Drugs That Prolong QT or Trigger Torsade de Pointes:
A heightened awareness of QT intervals and drug-induced arrhythmias may be one positive outcome of the hydroxychloroquine and azithromycin controversy.
Do You Care About Heart Arrhythmias?
If not, why not? Share your thoughts in the comment section below.

