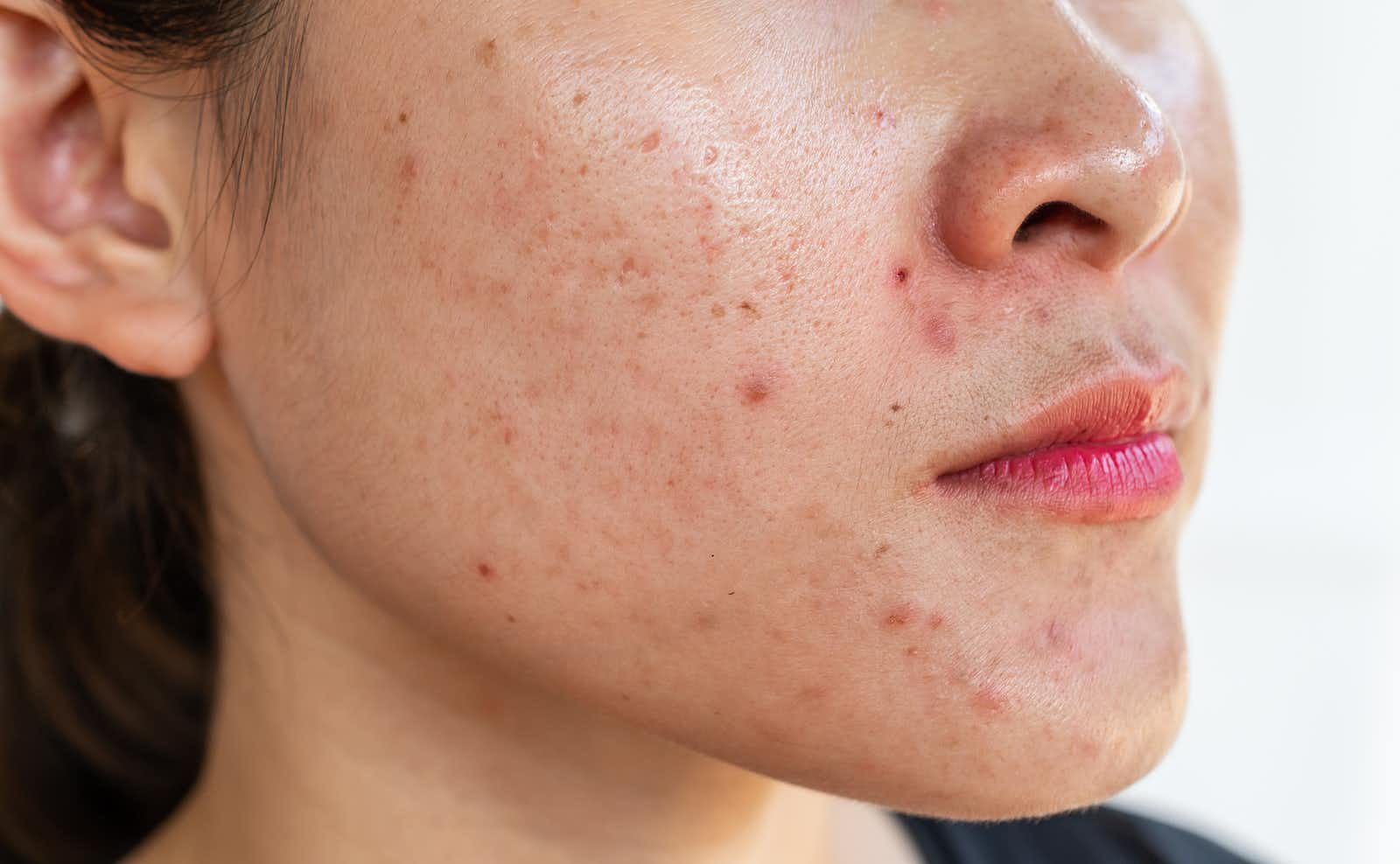
Acne is usually thought of as an adolescent problem, but dermatologists have been treating adults with blemishes for years. The technical term for such outbreaks of pimples is acne vulgaris. Common skin bacteria (mostly Propionibacterium acnes), the production of oils by the skin, and even the impact of hormones all seem to play a role in determining who gets acne and how severe it will be. When an oil-producing hair follicle becomes plugged up and the bacteria go to work feasting on the fatty acids trapped inside it, the body often reacts with inflammation. That’s what makes the pimple so sore and red.
How to Treat Acne:
Based on this scenario, there are four ways to tackle the problem of acne: discourage the bacteria, reduce the production of oil, control the hormones, or lower the level of inflammation. In practice, dermatologists mostly focus on bacteria and oil production. But perhaps trying to lower the level of inflammation is more practical than they think.
Blemishes are a common part of adolescence, but they also trouble many people well into adulthood. Changes in hormone levels seem to aggravate acne. Most treatments are aimed at killing or slowing down bacteria that are commonly present on and in the skin, and this usually works well until or unless the bacteria develop resistance. Stress seems to make acne worse (which is why college students have more zits during the week of final exams), but given the fact that stress is so hard to avoid, almost no treatments focus on controlling it. There are many approaches to acne treatment; if self-care does not prove effective, a dermatologist should be able to prescribe a therapy that will help.
Try a Low-Glycemic Index Diet:
Change your diet. A low-glycemic-index diet with very little sugar and other refined carbohydrates might improve skin significantly, and it will have other health benefits as well. Other things to avoid: milk and trans fatty acids, which are found in margarine and shortening. A study of dairy products and acne is currently under way.
Q. My 14-year-old daughter has had moderate acne for nearly two years. There are always five to ten small pimples on her forehead, and now she has ten to twenty pimples on her cheeks as well.
Clearasil left bleach stains on her clothes. Antibiotics the doctor prescribed didn’t help, and even seemed to make matters worse. The doctor suggested birth control pills but that seems ridiculous and it’s not an option we’d entertain.
Are there any topical or natural remedies that might work? What about diet?
A. Any link between acne and diet is controversial. Teens once were told to avoid chocolate and high fat foods. That turned out to be unhelpful.
Research published in the Archives of Dermatology (Dec, 2002) suggests, however, diet may make a difference. Populations on low-carb diets that don’t make blood sugar rise quickly may be less prone to blemishes. Your daughter might try avoiding foods like candy, cookies, French fries, potato chips, sugar and white flour to see if it helps her complexion.
A Facial Might Help:
Facial masks of clay may remove excess oil and help clear the skin. Other topical treatments include nutmeg mixed with milk or honey to make a paste for pimples. A tea tree oil gel (5 percent) is worth trying.
Clean Your Face, But Not with Soap:
Wash morning and evening with a gentle nonsoap cleanser such as Cetaphil or Cerave. Using a harsh or abrasive product may aggravate acne.
Apply Milk of Magnesia:
Although milk of magnesia is sold as a laxative to be taken internally, quite a few readers report that smearing it on the skin can help calm acne.
Q. I just started using topical MoM (milk of magnesia) on my skin and my acne has started shrinking. I am trying to get off oral antibiotics so I hope this remedy works.
A. Many readers tell us that applying milk of magnesia (magnesium hydroxide) to the skin can help clear up acne. The only reference we have found in the medical literature is a letter in the Archives of Dermatology (Jan. 1975).
Satisfied users apply it twice a day, leave it on for 10 or 20 minutes and then wash it off.
IL in Gilbert, AZ, offered this testimonial:
“You wrote about Milk of Magnesia as an acne remedy a couple of weeks ago. I am a 44-year old woman who has had acne (regular and cystic) since I was a teenager.
“When I was 18, I took Retin-A. It helped but did not clear it completely and you were correct about the side effects: depression, sensitivity to sun, redness in the face, cracked skin.
“My skin actually got better when I took birth control pills, but when I quit taking them, the acne resumed. My son (age 12) and I tried Milk of Magnesia after reading the article. We are having excellent results – not completely clear but really helping. It seems to slough off the skin and remove the redness. I have tried everything: Proactive, Retin A, Cleocin-T. etc. I have also taken countless antibiotics to no avail.”
Inquire About a Topical Antibiotic:
Ask your doctor about applying a topical antibiotic such as clindamycin or erythromycin. They can be helpful, but skin bacteria are developing resistance to these drugs.
Consider Retin-A:
Check with your doctor regarding a prescription for Retin-A. Be vigilant about protecting your skin from the sun or any other source of ultraviolet radiation while you are using this medicine.
Find Out About Nicomide-T:
Ask about Nicomide-T gel or cream. This vitamin-based topical medicine can reduce inflammation and may be almost as effective as some topical antibiotics.
Q. My son kept his acne under control with our dermatologist’s recommendation: niacinamide gel and a prescription topical Retin-A cream, alternating with benzoyl peroxide. The benzoyl peroxide and the niacinamide were over the counter.
The doctor said that niacinamide is an anti-inflammatory which often helps with skin conditions. When my son ran out for a week, the acne started coming back, so I know it really made a difference.
A. Acne often responds well to topical combination therapy. Tretinoin (Retin-A) was introduced over 40 years ago and remains a key acne treatment. Skin irritation, redness and sensitivity to sunlight are possible side effects.
Benzoyl peroxide can cause redness, burning, itching and peeling. Niacinamide (Nicomide-T) is a kind of B vitamin and does indeed have anti-inflammatory activity.
To learn more about acne in both teenagers and adults, you may find our eGuide to Acne Solutions of value. It describes an anti-acne diet and a variety of other treatments.
Oral Antibiotics May Be an Option:
Oral antibiotics may work even when topical antibiotics do not. Be sure to ask your doctor about side effects and interactions, and follow the dosing instructions carefully.
Birth Control Pills:
Women may benefit from birth control pills. Sometimes the diuretic spironolactone provides additional anti-acne power.
Isotretinoin Is Strong Medicine:
For severe acne that has not responded to other treatments, isotretinoin (Absorica, Myorisan, Zenatane) is an option. Discuss the risks and benefits thoroughly with your dermatologist before starting on a 5-month course of these pills. Because isotretinoin causes birth defects, women are required by the manufacturer to verify before taking any of this medication that they are not pregnant, and to confirm it again each month during treatment. They must also use two effective forms of contraception during the course of treatment.
Here is a reader’s experience:
Q. When I was 18 years old, I had severe acne. The dermatologist prescribed a type of vitamin A prescription.
It got rid of my acne within a few months. I then stopped taking the pills due to possible toxicity. My cousin had a similar experience. It felt like a miracle as the acne never returned.
Now my grandson is 18. He has very bad acne and the treatment is not yielding good results. How can we find a dermatologist who prescribes the pills we took, so he doesn’t throw his money away on unsuccessful treatments?
A. We suspect that the drug you are describing is isotretinoin. It was originally prescribed by the brand name Accutane. Although that brand is no longer available, dermatologists can still prescribe isotretinoin.
Because isotretinoin can cause birth defects if taken during pregnancy, it must be dispensed by a certified specialty pharmacy with precautions in place to prevent pregnant people from taking it. Another risk is severe depression.
Any dermatologist who treats severe acne should be familiar with isotretinoin. There are other treatments that may also be helpful. You can learn about them in our eGuide to Acne Solutions. We provide information about diet and home remedies as well as several prescription treatments.
Light Therapy Might Work:
Ask your dermatologist if Dusa Blue Light (photodynamic therapy) is appropriate for you. It should be administered by a dermatologist or plastic surgeon experienced with its use.

